Abstract
Background: Pulmonary vein isolation (PVI) is a cornerstone in atrial fibrillation (AF) treatment. Single-shot ablation devices are increasingly used due to their procedural simplicity. However, a direct comparison of newest-generation cyoballoon ablation (CBA) system featuring a variable diameter and the pentaspline pulsed field ablation (PFA) system is lacking.
Aim: To compare procedural efficiency, safety, and mid-term clinical follow-up of newest generation CBA with a pentaspline PFA catheter for PVI in patients with symptomatic AF.
Methods: This prospective, multicenter study enrolled patients treated with the newest generation CBA. Propensity score matching (1:2) was applied to compare these patients with those treated using PFA.
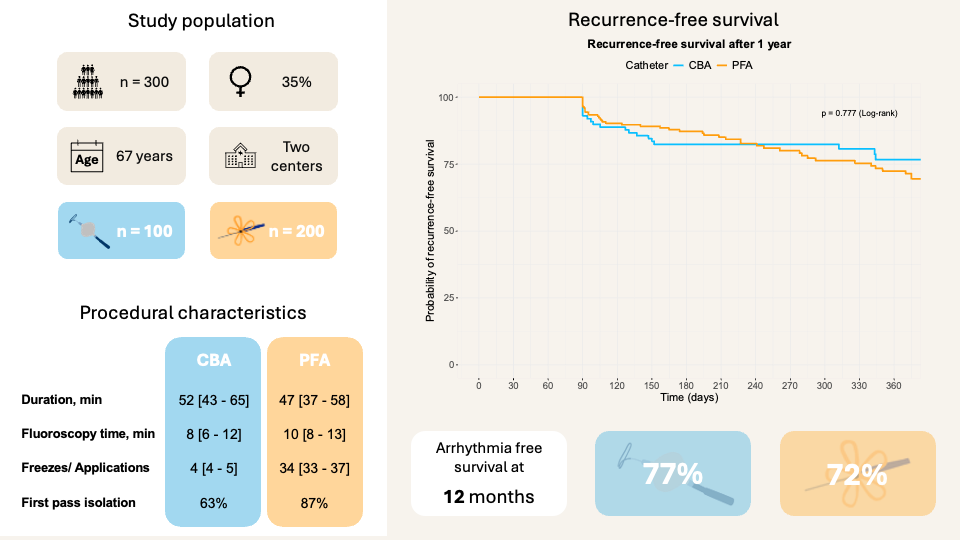
Results: Overall, 300 patients were included (age 67 [59 - 74] years, left ventricular ejection fraction 58% [51 - 62], left atrial diameter 41 mm [37 - 45], paroxysmal AF 156 (52%). Of these, 100 patients were treated with CBA and 200 patients with PFA. Median procedure duration was significantly longer in the CBA group (52 [43–65] min) compared to the PFA group (47 [37–58] min, p = 0.003). Fluoroscopy time was significantly shorter in the CBA group (8 [6–12] min) than in the PFA group (10 [8–13] min, p < 0.001). No differences in procedural complications were observed. At 1 year follow-up, recurrence-free survival was comparable between groups (CBA: 77% [95% CI 68%–87%] vs. PFA: 72% [95% CI 65%–80%], p = 0,777).
Conclusion: In this prospective, multicenter study, PFA demonstrated superior procedural efficiency with comparable efficacy and safety to newest-generation CBA for the treatment of AF.