Background: Approximately 50,000 patients in Germany suffer an embolic stroke of undetermined source (ESUS) each year. The significance of atrial cardiomyopathy (AtCM) in these patients is uncertain.
Methods: In this prospective AtCM study, patients with ESUS, AtCM (atrial fibrillation) and cardiac healthy individuals were analysed by means of laboratory, ECG and echocardiography. The patient groups were matched according to age and gender. Inclusion criteria were sinus rhythm at the time of the study. Exclusion criteria included severe valve stenosis or regurgitation, recent cardioversion, antiarrhythmic therapy, previous pulmonary vein isolation or cardiac surgery. The combined endpoint consisted of death and stroke. All patients with at least 1 year of follow-up were included in this preliminary analysis.
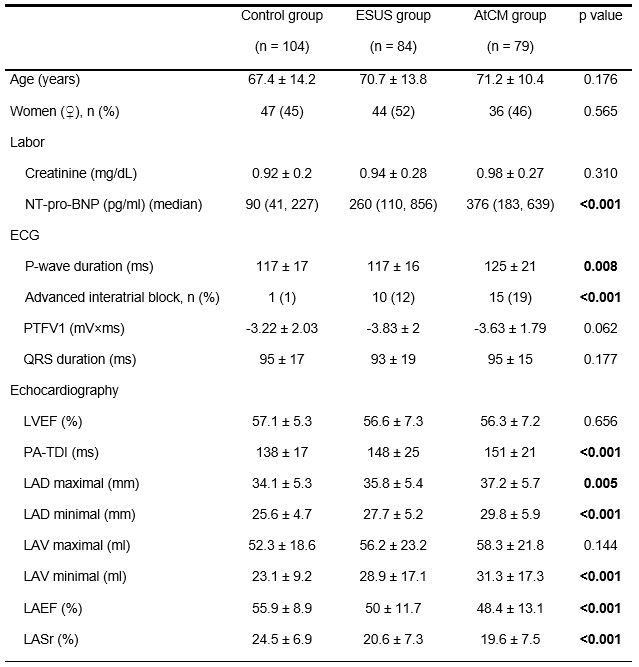
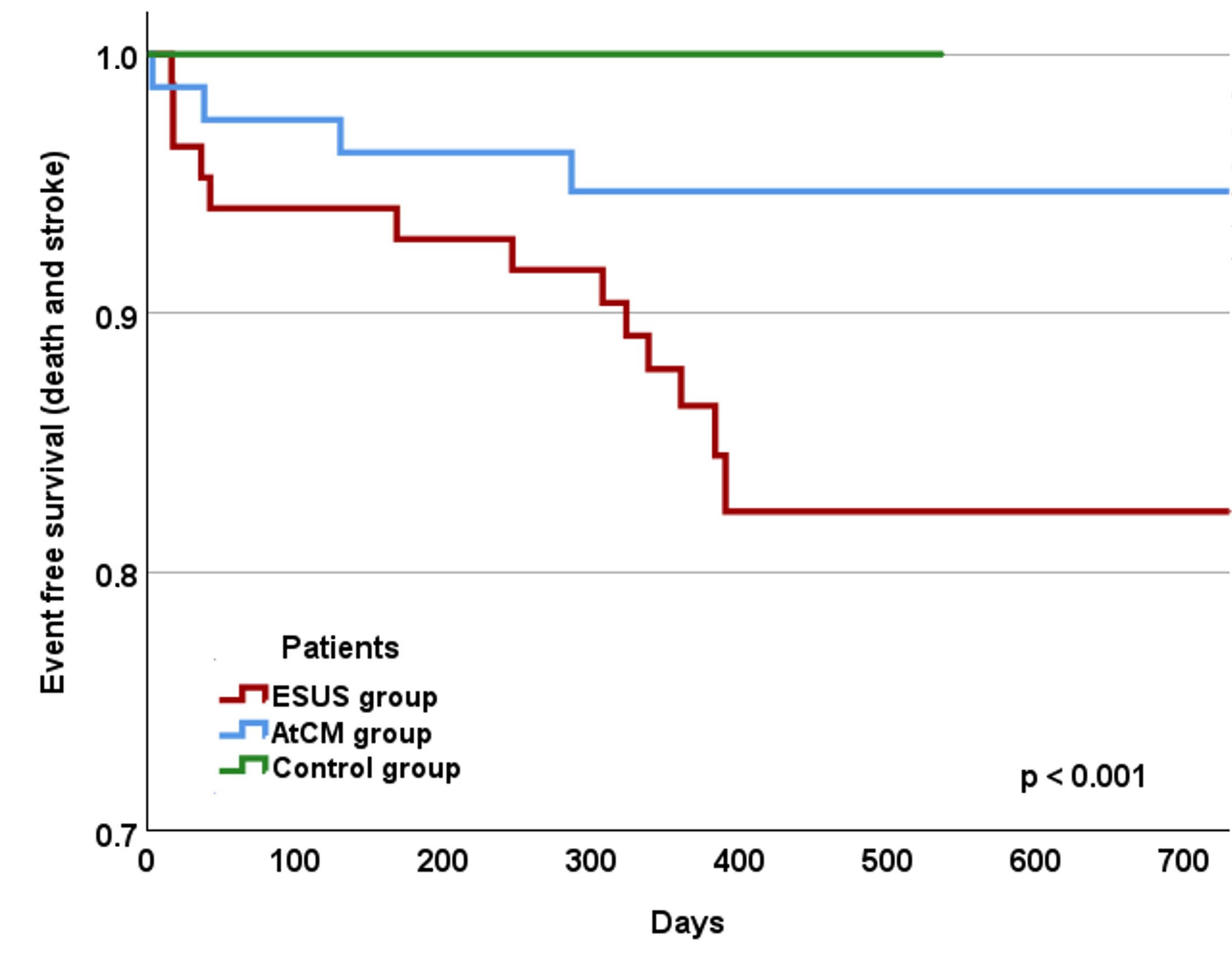
Results: A total of 267 patients (ESUS, n = 84; AtCM, n = 79; Controls, n = 104) were followed up for a mean period of 426 ± 202 days. Patients with ESUS had evidence of atrial cardiomyopathy with elevated NT-pro-BNP, larger left atrial diameter and volume, and lower left atrial reservoir strain than control patients (Table). During the first year, 11 patients (13 %) in the ESUS group suffered the endpoint (death, n = 1; stroke, n = 10) and 4 patients (5 %) in the AtCM group (death, n = 4). Patients in the control group did not suffer from any endpoints. The event rates differed significantly between the groups over the entire study period (Figure). In the ESUS group, 7 patients developed clinical atrial fibrillation (8%) over a mean period of 364 ± 239 days.
Independent predictors for the combined endpoint in the overall cohort were NT-pro-BNP > 420 pg/ml (HR 7.344; CI 2.338-23.066; p < 0.001), advanced interatrial block (HR 3.259; CI 1.147-9.260; p = 0.027) and LAD maximal ≥ 40 mm (HR 2.776; CI 1.093-7.048; p = 0.032).
Conclusion: This preliminary analysis demonstrates a high event rate in patients with ESUS. Compared to the control group, the ESUS group exhibits alterations in left atrial electrical activity and hemodynamics that are similar to those seen in the AtCM group. Our study suggests that parameters of atrial cardiomyopathy have prognostic significance.