Background: Survivors of out-of-hospital cardiac arrest (OHCA) frequently develop hypoxic-ischemic encephalopathy (HIE), which contributes to the persistently high in-hospital mortality. Semaphorin 3F (Sema3F), originally identified as an axon guidance molecule, has recently been implicated in pathophysiology after cardiac arrest and linked to survival. This study is the first to investigate the association between serum levels of Sema3F and neurological outcomes following OHCA.
Methods: In this prospective, two-center observational study, 59 adult patients with non-traumatic OHCA were enrolled. Blood samples were collected on admission (day 0) and on day 2 after return of spontaneous circulation (ROSC). Serum Sema3F concentrations were quantified using enzyme-linked immunosorbent assay.
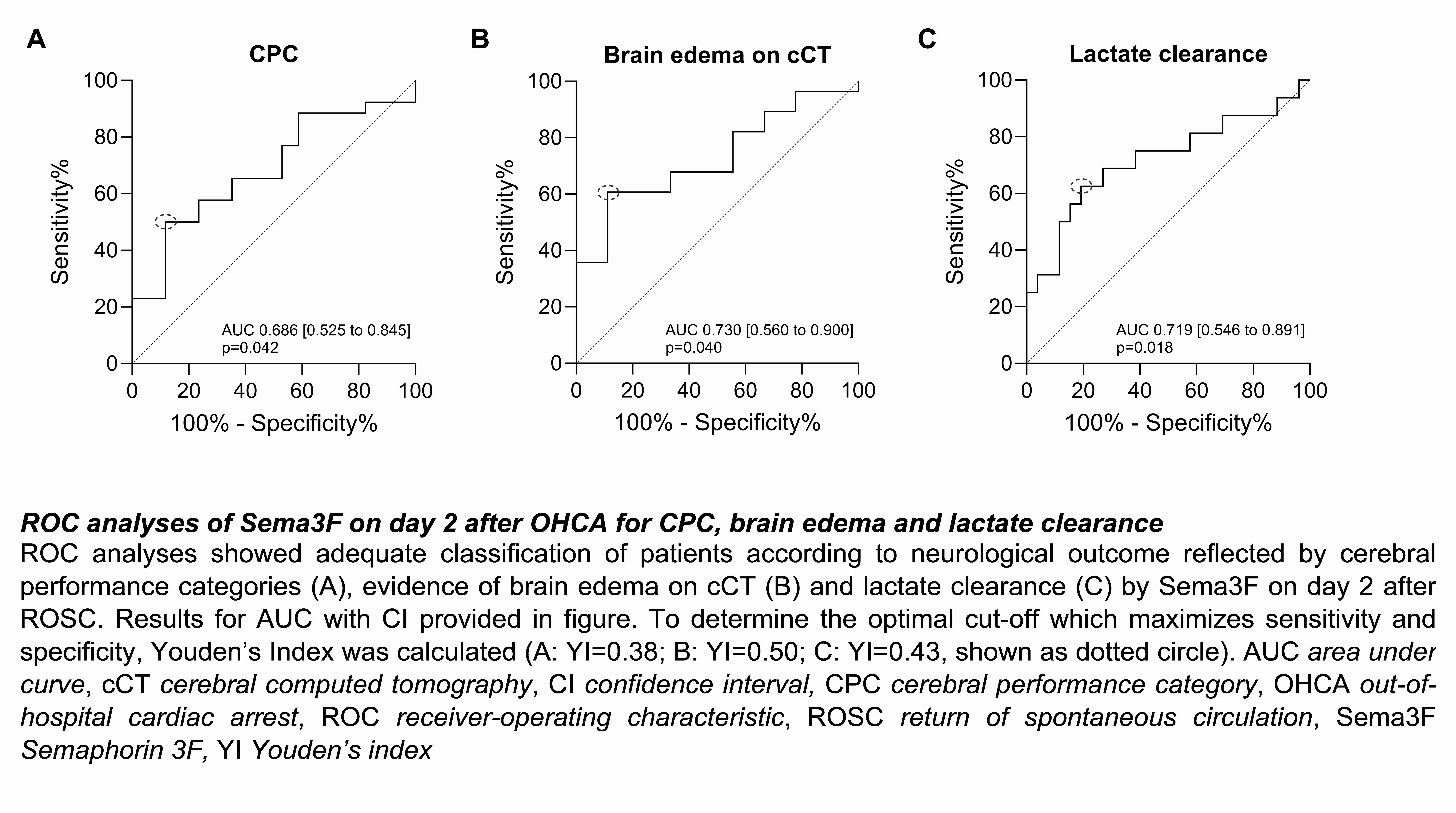
Results: Sema3F serum levels significantly increased from day 0 to day 2 after ROSC (day 0: 41.91 [26.56-67.89] vs. day 2: 60.98 [34.10-142.14] ng/ml, p=0.004). Elevated day 2 Sema3F levels were associated with unfavorable neurological outcome (Cerebral Performance Categories 3-5, p=0.015) and with cerebral edema on cranial computed tomography (p=0.040). Moreover, higher Sema3F concentrations on day 2 correlated with inadequate lactate clearance, a surrogate marker of poor neurological outcome (p=0.002). No relationship between Sema3F and NSE on day 2 after ROSC was observed (r=0.136 p=0.475). ROC analysis showed acceptable discrimination of Sema3F for unfavorable neurological outcome (AUC=0.686, p=0.042) and moderate performance for cerebral edema (AUC=0.730, p=0.040) and impaired lactate clearance (AUC=0.719, p=0.018). A cut-off for Sema3F on day 2 >114.5 ng/ml was identified for predicting poor neurological outcome.
Conclusion: Elevated serum Sema3F levels on day 2 after OHCA are associated with cerebral edema, poor neurological outcome and impaired lactate clearance. These findings suggest that the axon guidance molecule Sema3F may play a role in brain injury following non-traumatic cardiac arrest.