Background: The ratio between basal right and left ventricle diameter (RV/LV) measured on contrast enhanced Computertomography (CT) is routinely used in the diagnosis of acute pulmonary embolism (PE). An RV/LV ratio ≥ 1.0 has been shown to reliably indicate right ventricular strain and predict adverse outcomes. The relationship between thrombus volume (TV) and thrombus surface area (TSA) to RV/LV ratio remains unclear.
Objective: The aim of this study was to investigate whether the CT-derived RV/LV ratio correlates with TV or TSA in 102 patients with acute intermediate-high risk PE.
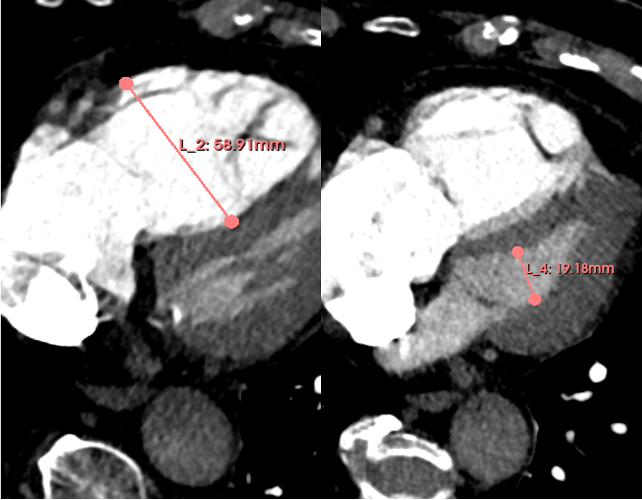
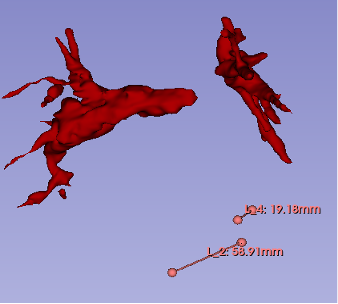
Methods: We conducted a retrospective analysis of 102 CT scans (Siemens-Sensation 128) of patients diagnosed with acute intermediate-high risk PE between 2019 and 2025, as recorded in the Chemnitz PE Registry (CLoT). RV/LV ratio was measured in the axial plane at the largest diameters of the right and left ventricles (Figue 1). TV and TSA were quantified using the software platform for medical image processing “3D Slicer” (Version 5.8.1;Figure 2). For statistical analysis patients were divided in 4 groups by quartiles (Q) based on their mean RV/LV-Ratio. Spearman rank correlation and Kruskal-Wallis-Tests were used to evaluate associations between RV/LV ratio and TV or TSA. Statistics was done with R using Rstudios.
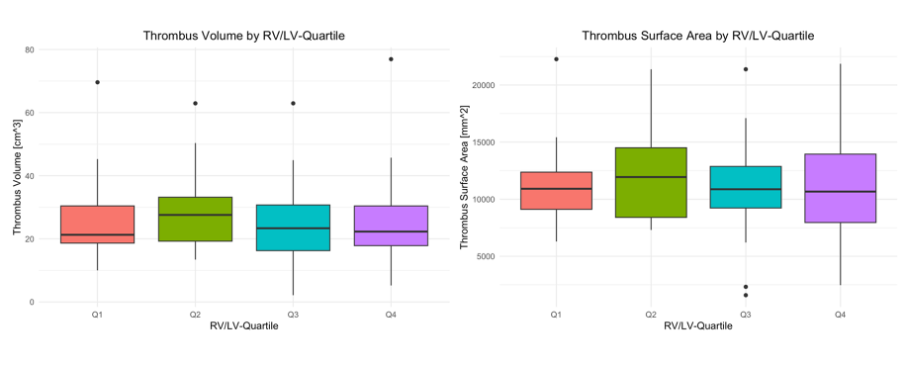
Results: A total of 148 patients with intermediate-high risk PE were screened, of whom 102 were included in this study. Despite RV/LV no relevant differences in baseline charcteristics were observed. The mean RV/LV ratio differed in subqroups (Q1:1,24; Q2: 1,52; Q3: 1,77; Q4: 2,25). Between quartiles no significant difference for TV and TSA were observed (TV: p = 0,67; TSA: p = 0,69)(Figure 3). No correlation was observed between TV (rho = 0.086; p = 0.861), TSA (rho = 0.017; p = 0.867) and RV/LV ratio.
Conclusion: In this study, no correlation between RV/LV ratio and TV or TSA was observed, not even between the highest and lowest quartile. The cause of right heart strain in patients with intermediate-high risk PE goes beyond thrombus volume and surface area. Especially considering the main goal in interventional therapies – reducing thrombus burden - future prospective studies should aim to examine the role of thrombus characteristics or other cause in therapeutic decision-making.
