Introduction: Atrial fibrillation (AF) is the most common arrhythmia, driven by proarrhythmic remodeling including processes that promote enhanced ectopic activity, altered conduction, and a reentry-prone substrate. Cardiometabolic diseases, such as Diabetes mellitus, are associated with an increased risk for AF, but the specific underlying mechanisms are largely unknown. SGLT2 inhibitors are established treatments for diabetes. Recent data suggest that SGLT2 inhibitors may also have antiarrhythmic effects, yet the cellular mechanisms remain incompletely understood.
Objective: We aimed to investigate the antiarrhythmic effects of SGLT2 inhibitor treatment (dapagliflozin 10 mg/d) in genetically modified diabetic swine.
Methods: We studied atrial conduction properties and arrhythmia susceptibility in an INSC94Y transgenic swine model for diabetes using ECG, invasive electrophysiology and atrial burst pacing. Subsequently, we evaluated the treatment effects of dapagliflozin in this pig model. Non-diabetic wildtype littermates served as control animals. Furthermore, we analyzed the distribution of Cx43 in atrial tissue. Additionally, human atrial tissue samples were obtained from the LMU hospital’s biobank, after approval by the hospital’s ethics committee and written informed consent by the patients prior to study participation.
Results: Diabetes leads to higher susceptibility for AF, whereas treatment with dapagliflozin protects from AF inducibility (Fig. 1A-B). P wave duration and interatrial conduction time are shortened in diabetic INSC94Y swine compared to non-diabetic wildtypes (Fig. 1C-D). Dapagliflozin treated animals show normalized P wave duration and interatrial conduction time. Lateralization of Cx43 is elevated in the atria of diabetic INSC94Y pigs (Fig. 1E). Dapagliflozin treatment mitigates lateralization of Cx43 in INSC94Y pigs (Fig. 1E). Similar effects on Cx43 localisation were also seen in human atrial tissue (Fig. 1F).
Conclusion: Diabetes mellitus leads to increased susceptibility for AF in a translational pig model by affecting atrial conduction properties driven by elevated Cx43-lateralization. Notably, treatment with dapagliflozin prevents Cx43 upregulation and lateralization, normalizes atrial conduction and thus, protects against AF inducibility. However, future studies are warranted to fully unravel the complex relationship between AF and diabetes.
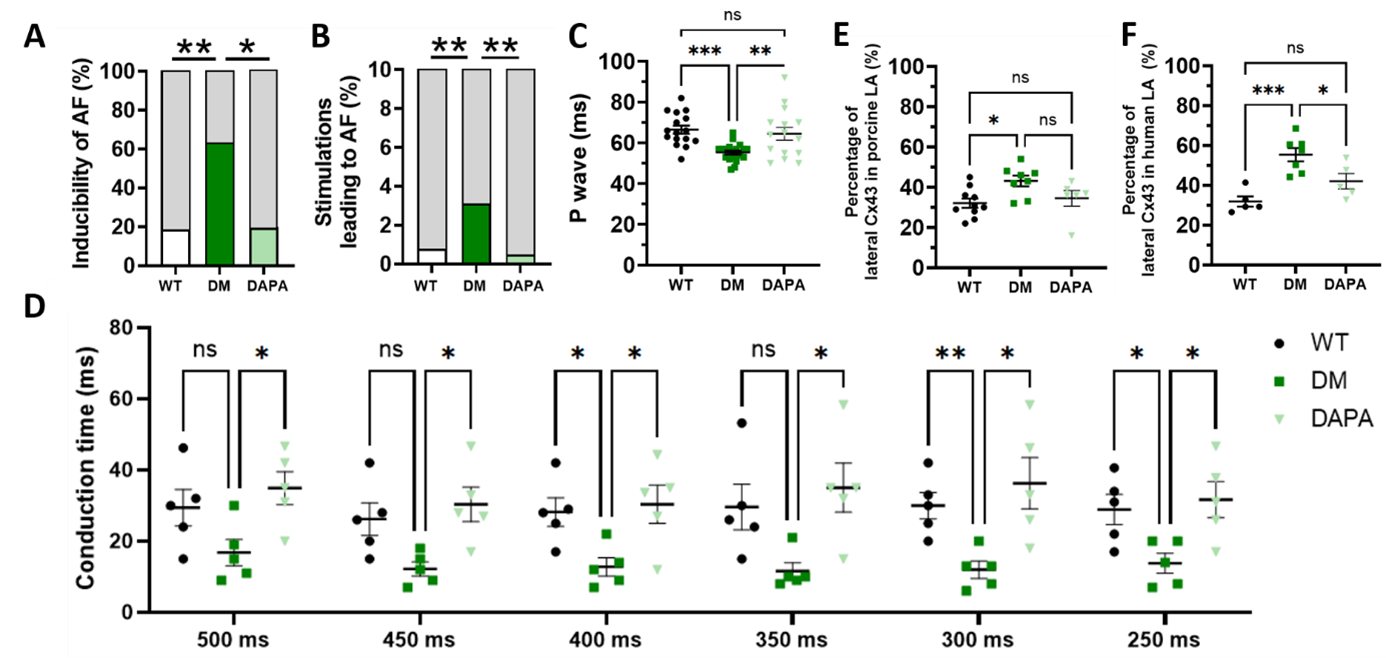
Figure 1: (A-B) Inducibility of atrial fibrillation (AF) in non-diabetic wildtype (WT), diabetic (DM) and dapagliflozin-treated (DAPA) INSC94Y swine shown as percentage of pigs with AF (A) and percentage of burst pacing stimulations that led to an AF episode (B). (C) P wave duration (ms) measured in WT, DM and DAPA swine. (D) Interatrial conduction time (ms), measured between the distal and proximal electrode of the stimulation catheter, at different pacing cycle lengths. (E) Percentage of lateral oriented Cx43 in porcine samples of the left atrium (LA). (F) Percentage of lateral oriented Cx43 in human samples of the left atrium.
