Introduction: Chest pain is often the most important symptom in patients with acute myocardial infarctions. However, previous studies have shown, that especially women are less likely to present with typical chest pain compared to men, which might explain their worse prognosis. Aim of the present study was to assess, how gender affected the likelihood of chest pain (CP) in patient cohorts stratified by age and gender and whether lack of chest pain had an impact on prognosis.
Methods: All patients, admitted with STEMI to a large German PCI center between 2006 and 2022, were analyzed. Patients were assigned to those with chest pain (CP) and without chest-pain (No-CP) and stratified by age into three groups: <60 yrs. (A1), 60-79 yrs. (A2), ≥80 yrs. (A3).
Results: Of a total of 11655 STEMI-patients included in this study, 10553 (90.5%) presented with chest pain (CP), while 1102 (9.5%) did not (No-CP). Rates of No CP were higher in women compared to men (12.0% vs. 8.5%, p<0.01). When stratifying by age, two observations could be made: First, No-CP rates increased with age and second, only in the elderly female sex was associated with higher No-CP-rates (table). No-CP was associated with a higher likelihood of cardiogenic shock (50.9% in No-CP vs. 10.3% in CP, p<0.01) and was associated with higher rates of a reduced left-ventricular ejection fraction post STEMI: LV-EF<40% in No-CP: 28.8%, CP: 13.3%, p<0.01. Univariate comparison showed a marked increase in 30-day-mortality in No CP vs. CP: 35.1% vs. 8.1%, p<0.01. In a Cox regression model (adjusted for age, diabetes, multi-vessel-disease, interventional success, peak CK) No-CP was associated with a significantly higher 30-day-mortality: HR 4.5, 95% CI 3.9-5.4, p<0.01. The disadvantage for No-CP remained when excluding all patients with cardiogenic shock from the analysis: HR 2.29, 95% CI 1.6-3.9, p<0.01. When stratifying by age, the negative impact of No-CP on 30-day-outcome remained significant in all age strata (figure).
Figure: Distribution of No-CP by age group and sex and impact of No CP on 30-day-mortality
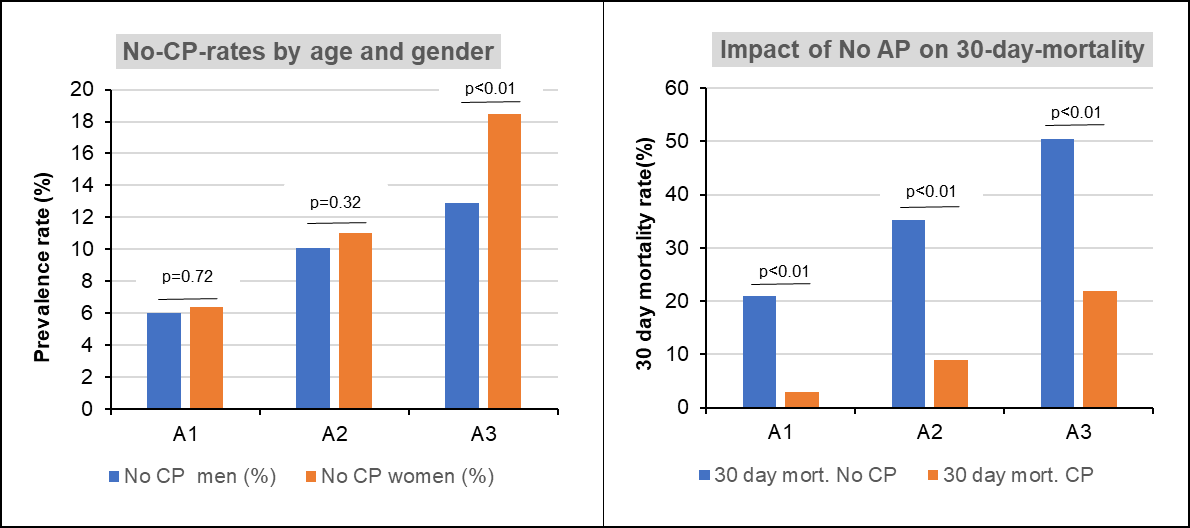
Conclusions: In this analysis of patients with STEMI, lack of chest pain was more frequent in women, however, when stratifying by age, a significant difference could only be observed in the elderly. Independent of sex distribution, lack of chest pain was associated with higher rates of cardiogenic shock, post STEMI-complications and a markedly worse 30-day-outcome. Chest pain could therefore be interpreted as a protective warning signal in the context of acute myocardial infarctions.
