Introduction: Acute pulmonary embolism (PE) remains a significant cause of morbidity and mortality worldwide, with rising incidence rates posing ongoing challenges to healthcare systems. Our study focused on hospitalised patients diagnosed with acute PE and examined haemodynamic stability, treatment patterns, and associated in-hospital mortality rates across different age groups in Germany.
Methods: Using the German Analysis Database for Evaluation and Health Services Research (DADB), we conducted a retrospective analysis of health claims data from 2014 to 2023, including approximately 4 million individuals. Patients with a hospital diagnosis of PE were included in the study. Haemodynamic stability was defined as the absence of cardiopulmonary resuscitation or shock during hospitalization.
Results: We identified 23,895 patients accounting for 28,404 hospitalisations with a diagnosis of PE. The incidence of PE increased from 73 per 100,000 in 2014 to 102 per 100,000 in 2023. The median age was 67 years (IQR 56-78) and the median hospital stay was 8 days (4-15). Cancer was reported in 21.5% of the cases, and 18.0% underwent surgery during hospitalisation. Systemic thrombolysis was administered in 3.8% of cases and was most frequently used among patients aged 20–29 years (6.5%). Embolectomy was performed in 0.7 % of the patients and was most common in the 30–39-year age group (1.0%). Both treatment options were used less frequently with increasing age. Over the study period, the use of systemic thrombolysis remained stable, whereas embolectomy peaked in 2022 (1%). The risk of in-hospital mortality increased with age (Figure 1). Among the 3,101 haemodynamically unstable patients, 1,341 (43.2%) died in the hospital. In contrast, in the population of 25,303 haemodynamically stable patients, 1,651 (6.5%) died in the hospital. A detailed comparison between survivors and non-survivors is presented in Table 1.
Conclusion: In this large nationwide analysis, the incidence of acute pulmonary embolism increased substantially over the past decade. Treatment patterns and outcomes varied by age. Despite advances in diagnosis and management, in-hospital mortality remains high, particularly among haemodynamically unstable and older patients. The use of systemic thrombolysis and surgical embolectomy remains limited and declines with age. These findings underscore the need for improved risk stratification and targeted therapeutic strategies to enhance survival in patients with acute PE.
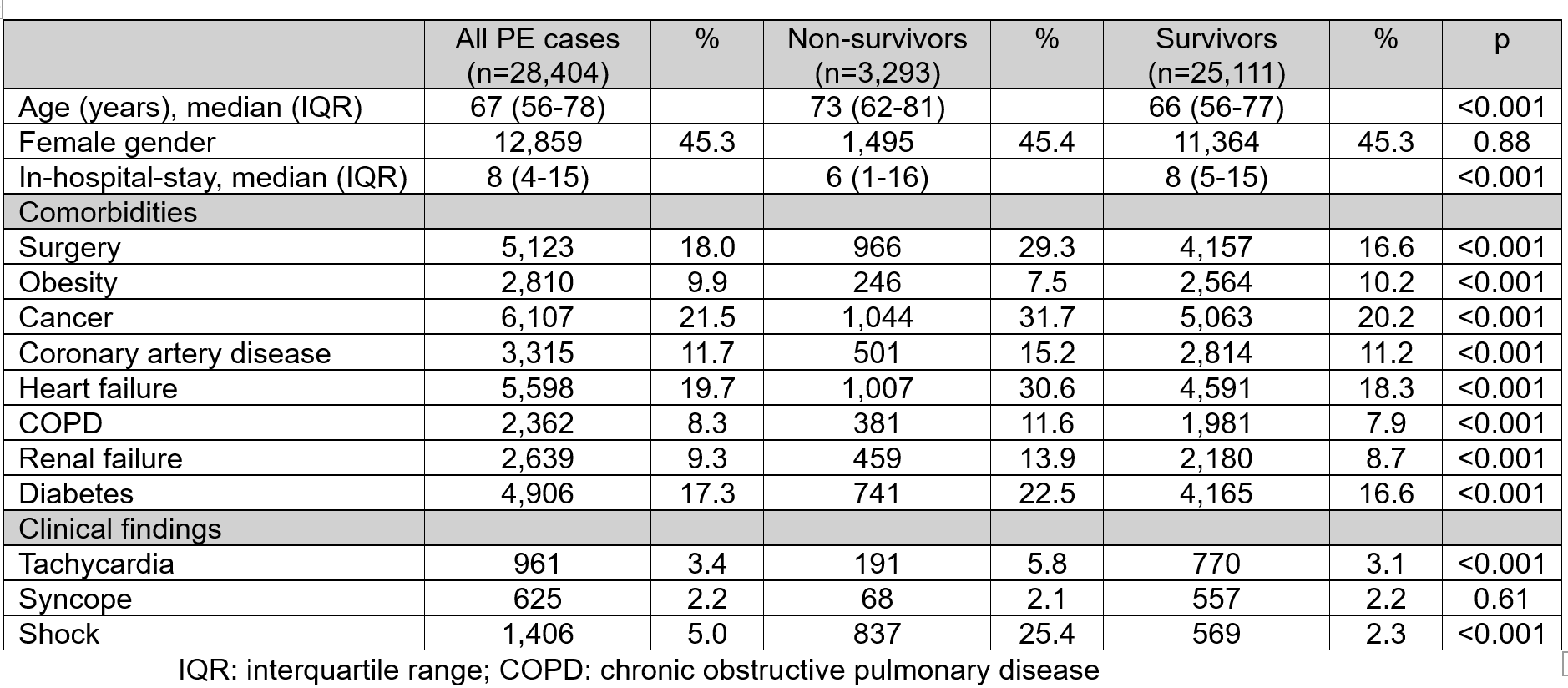
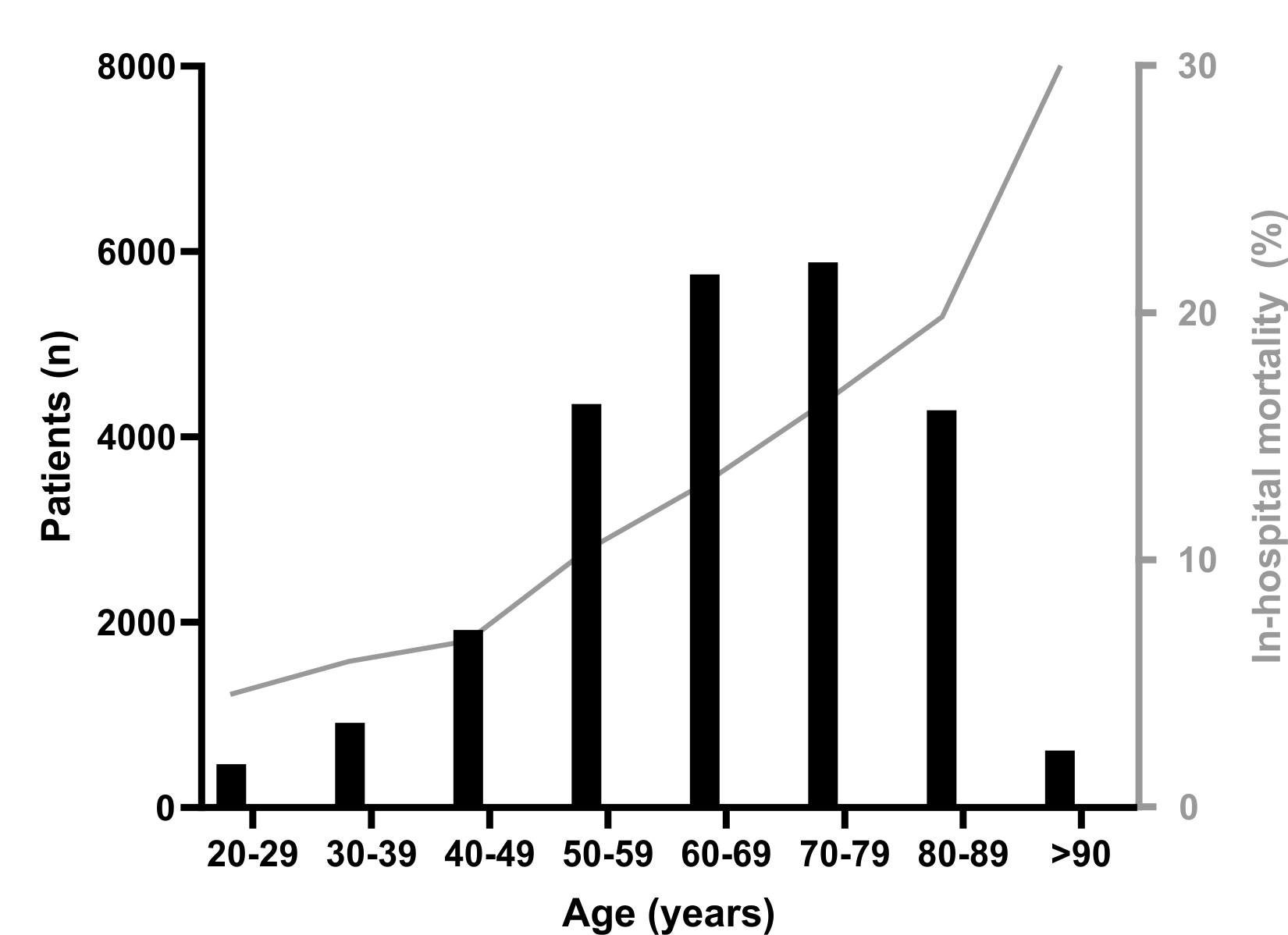
Figure 1 Prevalence (black bars) and in-hospital mortality rate (grey line) according to age
