Background: Atrial fibrillation (AF) is a leading cause of cardiovascular morbidity and mortality worldwide. Genome-wide association studies (GWAS) have identified variants in the Meis1 locus associated with prolonged PR interval and increased AF risk in patients. Despite these genetic associations, the role of Meis1 in atrial electrophysiology and arrhythmogenesis remains poorly defined.
Objective: This study aims to uncover the functional role of Meis1 in cardiac electrophysiology, arrhythmogenesis and autonomic nervous system regulation.
Methods: Invasive electrophysiology (EP) assessed atrial conduction, nodal function, and arrhythmia susceptibility in Balb/c mice with or without MEIS1 inhibition. Implantable telemetry monitored ECG, spontaneous arrhythmias, and heart rate variability in freely moving awake mice. Masson’s trichrome staining evaluated histopathological changes across cardiac compartments.
Results: Balb/c mice were randomly assigned to control (saline i.p.) or MEIS1-inhibition group (100 µM MEIS1 inhibitor i.p.). EP data revealed that MEIS1 inhibition significantly increased atrial arrhythmia inducibility accompanied by a prolonged atrial effective refractory period and delayed sinus node recovery time (n=18-24 mice). Implantable telemetry monitoring showed that MEIS1 inhibition did not affect overall spontaneous arrhythmia burden compared with saline-treated mice (n=4 mice per group). Heart rate variability (HRV) analysis demonstrated autonomic alterations, characterized by a reduction in heart rate, prolonged PR intervals and elevated RMSSD (Root Mean Square of Successive Differences) values, indicating autonomic imbalance. Furthermore, Masson's trichrome staining confirmed absence of atrial fibrosis (n=3-4 mice).
Conclusion: In summary, MEIS1 inhibition induces autonomic remodeling and electrical instability without structural changes, revealing MEIS1 as a key modulator of atrial arrhythmogenesis.
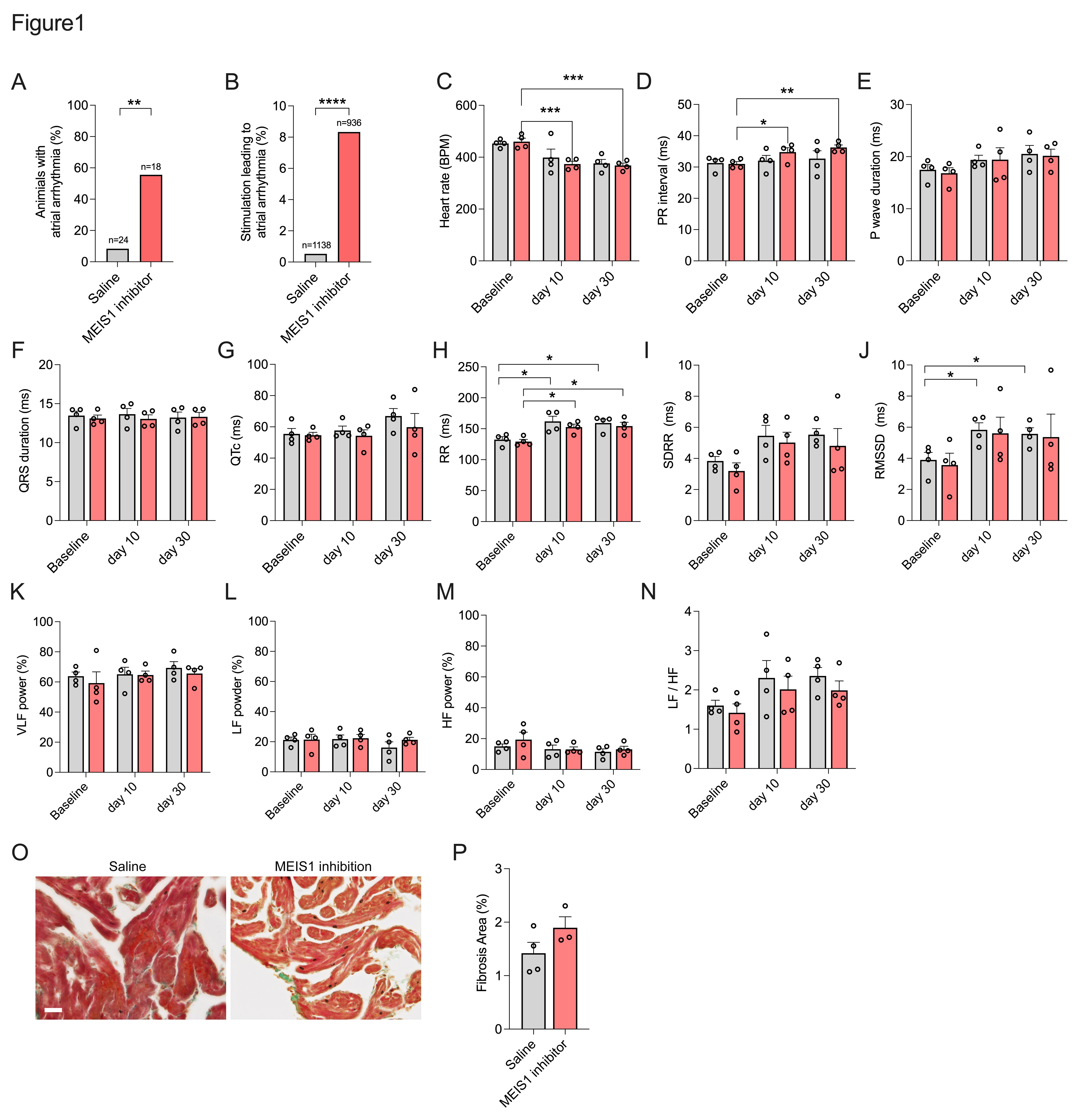
Figure 1. MEIS1 inhibition increases atrial arrhythmia inducibility and alters autonomic regulation. (A-B)Inducibility of atrial arrhythmias shown as percentage of stimulations resulting in arrhythmias >1 s (A) and percentage of mice with arrhythmias (B) in mice treated with saline (n=24) or MEIS1 inhibitor (n=18). (C-G) ECG parameters including heart rate (C) PR interval (D) P-wave duration (E) QRS duration (F) and QTc (G) in saline-treated (grey) and MEIS1-inhibited (pink) mice (n=4 per group). (H-N) HRV parameters, including median RR interval (H)standard deviation of RR intervals (SDRR) (I) RMSSD (J)percentage of very-low-frequency (VLF, 0.15-0.50 Hz) oscillations (K) percentage of low-frequency (LF, 0.15-1.50 Hz) oscillations (L) percentage of high-frequency (HF, 0.15-1.50 Hz) oscillations (M) and LF/HF ratio (N) in saline-treated (grey) and MEIS1-inhibited (pink) mice (n=4 per group). (O) Representative images of Masson‘s staining in the right atrium and (P) quantification of fibrotic area in both groups (saline group, n=4; MEIS1 inhibitor group, n=3). *p<0.05, **p<0.01, ***p<0.001, ****p<0.0001 by student t test or two-way ANOVA with Tukey‘s multiple-comparison test.