Background
The recently identified structure, known as the left-sided atrial septal pouch (LASP), has emerged as a potential cardiac source of thromboembolic events (SOE) and has attracted considerable interest within the medical community. In this study, we aim to evaluate the characteristics of patients with LASP thrombosis.
Methods
We retrospectively reviewed echocardiographic data from patients who underwent transoesophageal echocardiography (TOE) at the University Hospital of Jena between September 2015 and August 2025. Images were analysed offline by a single investigator (A.H.) using the TomTec® Image-Arena platform. LASP was identified as a kangaroo-like pouch, indicating partial fusion of the septum primum and septum secundum within the left atrium. Patent foramen ovale was excluded in all cases with a contrast study. Clinical data and patient outcomes were systematically assessed (see Figure 1).
Results
From an echocardiography database of over 100,000 studies, 11 patients diagnosed with TOE were identified. Except in the case of extremely large lesions (which was observed only once), LASP thrombosis was identifiable solely by TOE. Most patients were male (81.8%) with a median age of 74.2 years ; permanent atrial fibrillation occurred in 81% and mean ejection fraction was 40.4%. Common findings included left atrial dilation and high-grade "smoky" echoes (seen in ~90%), as well as occasional thrombus in the left ventricle and appendage. Clinical presentations were mainly TIA or ischemic stroke (50%); one patient had acute lower limb ischemia. Two pts. underwent cardiac surgery, with one requiring intraoperative femoral artery embolectomy for new embolism. Four patients were lost to follow-up. One-third of the patients died from either cardiac or non-cardiac causes.
Conclusion
Our findings indicate that: 1) While infrequent, the LASP as a potential nidus for thrombus formation is likely under-diagnosed, and clinicians—including Heart-Brain teams—should actively consider it as a potential SOE, a “second atrial appendage"; 2) Definitive diagnosis requires contrast TOE. Further prospective, multi-centre studies are warranted.
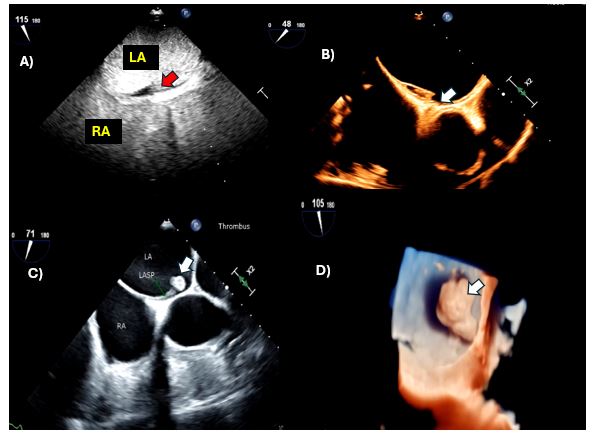
Fig. 1 illustrates distinct morphologies of LASP thrombi as revealed by ultrasound enhancing agents (pane A), as well as by two-dimensional (Panel B-C) and three-dimensional echocardiography (Panel C). Arrows indicate thrombus
