Background: Lipoprotein(a) (Lp[a]) has been recognised as a critical biomarker due to its association with atherosclerotic cardiovascular disease (ASCVD). For statin-treated individuals, the risk linked to elevated Lp(a) levels and potential adjusted thresholds remains insufficiently defined.
Aim: The aim of this analysis was to evaluate whether Lp(a) serves as an independent risk factor for further risk stratification in a population treated with statins, and whether existing thresholds for elevated Lp(a) are adequate for these high-risk patients.
Methods: The analysis included 17,376 patients aged ≥ 45 years with either established ASCVD or type 2 diabetes (T2DM) from the UK Biobank. We compared cardiovascular (CV) endpoints between low-Lp(a) cohort and high Lp(a)-cohort. Rather than using established clinical thresholds, we defined these groups based on the lower and upper tertiles of the Lp(a) distribution in our study population. This yielded a cutoff of 46.8 nmol/L for the upper tertile, while patients with Lp(a) <12.5 nmol/L were assigned to the lower tertile. Endpoints included hospitalization due to myocardial infarction (MI), unstable angina pectoris (AP), stroke, and ASCVD (MI, stroke, AP), as well as coronary revascularization. Additional endpoints were the composite of major adverse cardiovascular events (MACE), all-cause mortality, and CV mortality. Incidence rates were calculated using a generalized linear regression model with a Poisson log-link and observation time as the offset variable, adjusting for confounders age, sex, smoking status, body-mass-index (BMI), T2DM, arterial hypertension (AHT), fair skin-color, and non-HDL cholesterol.
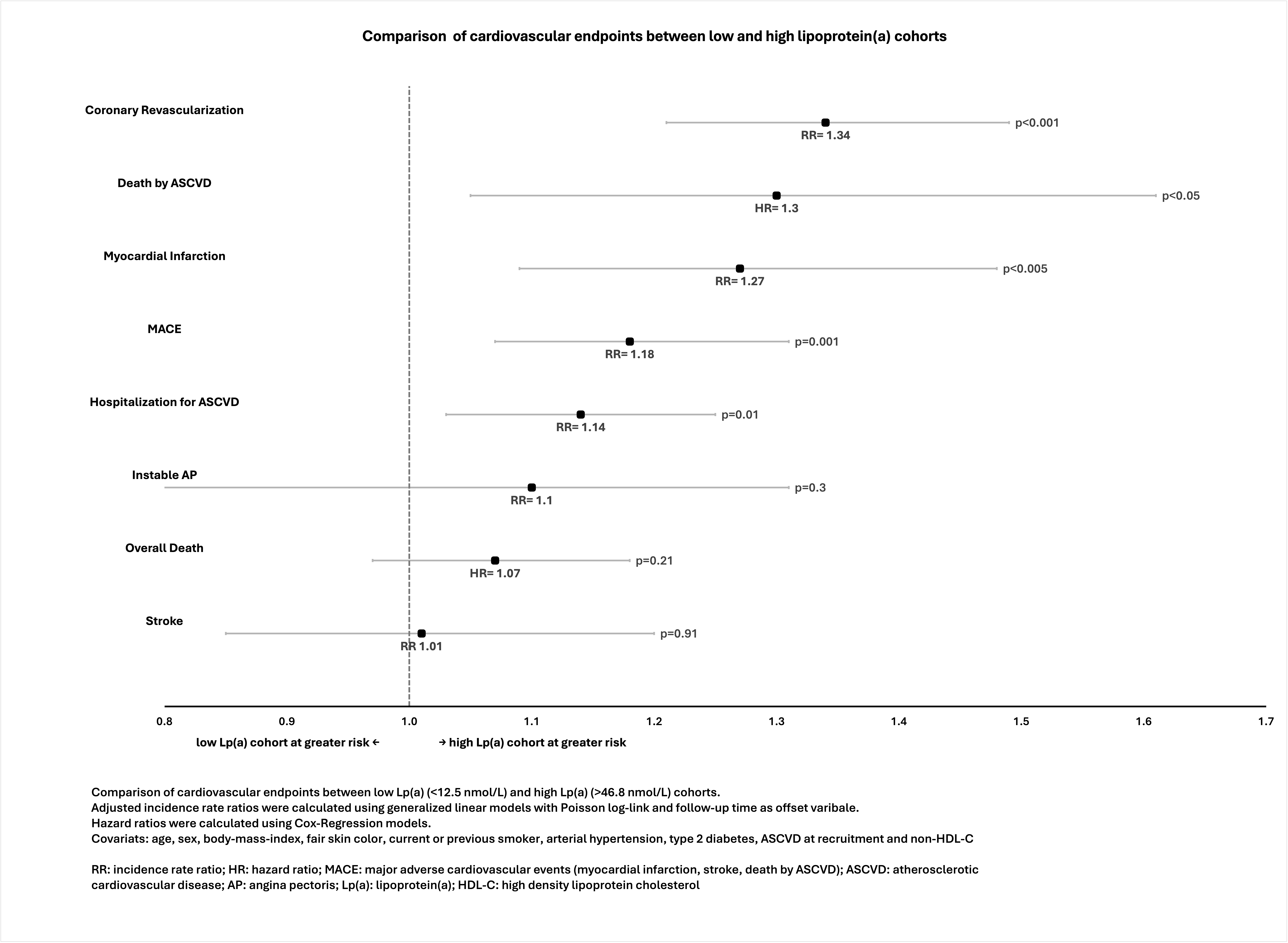
Results: Individuals with elevated Lp(a) levels above 46.8 nmol/L showed a 14% higher hospitalization rate for ASCVD (p < 0.05), a 27% higher hospitalization rate for MI (p < 0.01), a 34% higher rate of coronary revascularization (p < 0.001), and an 18% higher MACE rate (p < 0.001). ASCVD-related deaths occurred 30% more frequently in individuals with high Lp(a) compared to those with low Lp(a) levels.
Conclusion: In a population at high CV risk, even moderately elevated Lp(a) levels above 46.8 nmol/L were associated with a significantly increased risk of CV events. This contrasts with the prevailing assumption that Lp(a)-related CV risk becomes clinically relevant only above 105 nmol/L. In high-risk patients, Lp(a)-associated events may therefore emerge at levels notably lower than previously assumed. These findings highlight the importance of Lp(a) as an independent ASCVD risk factor, even in statin-treated individuals, and suggest that this particularly vulnerable population may require lower Lp(a) thresholds to more accurately characterize residual CV risk.