Background
Statin intolerance (SI) represents a major limitation in managing cardiovascular risk. Affected patients face an increased likelihood of adverse cardiovascular outcomes and have significantly lower quality of life. Patients with SI may have distinct beliefs about medicines, which may impact adherence and lipid management, representing a potential target for educational interventions.
Methods
The Statin Intolerance Registry (NCT04975594) is a multicenter observational study at 19 German sites, enrolling 1,124 patients with SI between 2021 and 2023. SI was defined as intolerance to at least two different statins with symptom improvement after statin dose reduction or discontinuation. Baseline assessments included the “Beliefs about Medicines Questionnaire” (BMQ). Results were compared with published data from chronic disease patients treated in general practice in Germany (Mahler et al., J Eval Clin Pract 2012;18:409–413). The necessity-concerns differential (NCD) was calculated as the difference between the BMQ “necessity” and “concerns” subscales. A positive score indicates the perceived necessity outweighs medication-related concerns, whereas a negative score reflects a more skeptical attitude towards medication.
Results
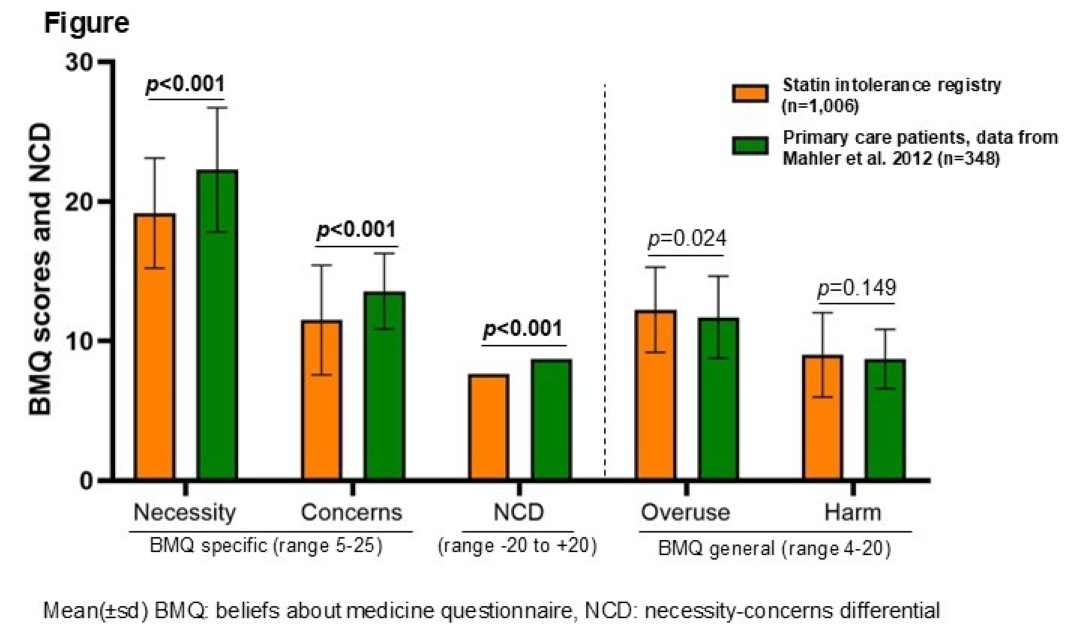
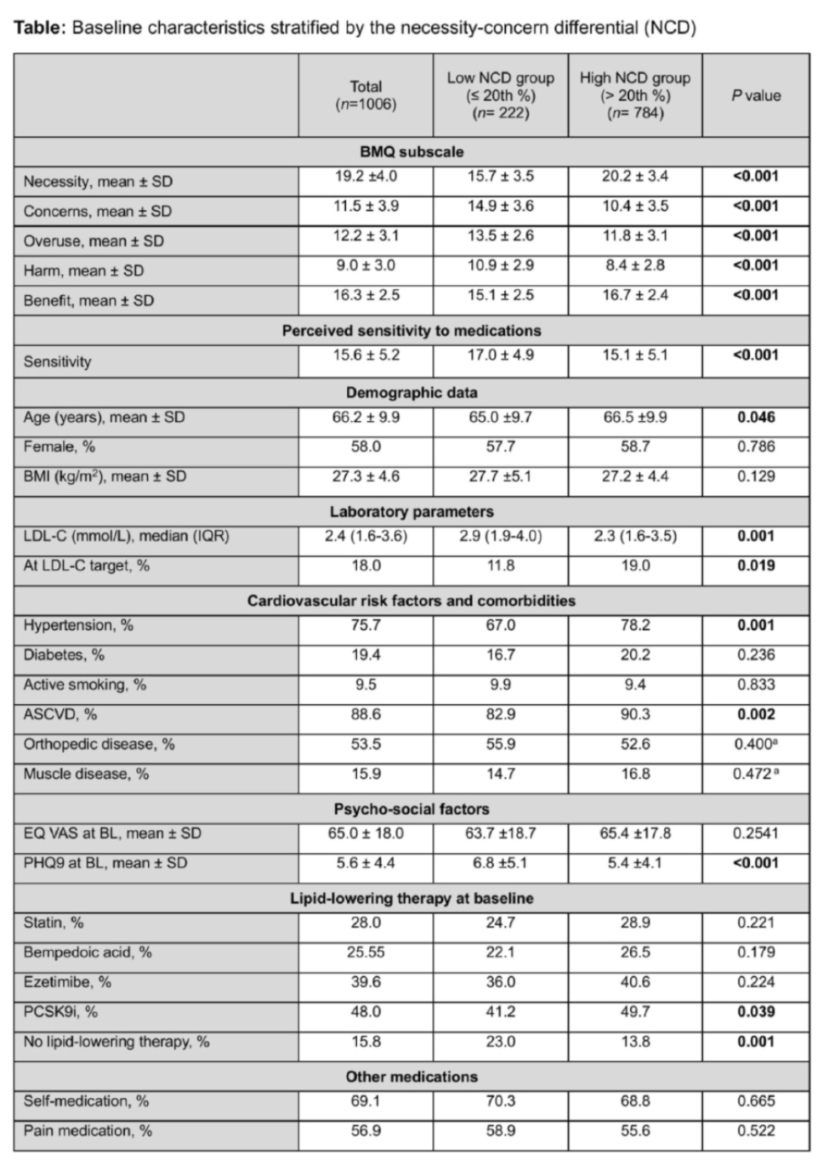
A total of 1,006 patients with SI (58% female, mean age 66.2 [SD 9.9] years) were analyzed. Among patients with SI, those with a low NCD (≤20th percentile) compared to those with an NCD >20th percentile were less likely to take lipid-lowering therapy (patients on therapy: 77% vs. 86.2%, p<0.001), had higher LDL-C levels (2.9 vs. 2.3 mmol/l, p=0.001), and were less likely to achieve the LDL-C target (11.8% vs. 19.0%, p=0.019). Patients with a low NCD scored higher on the BMQ domains “harm” and “overuse”, indicating stronger beliefs regarding adverse effects of medication. Compared with patients with chronic diseases in general practice, patients with SI showed significantly lower BMQ scores for the domains “necessity” (19.2 vs. 22.3, p<0.001) and “concerns” (11.5 vs. 13.6, p<0.001). Although these subscores were both lower in SI patients, the NCD was also significantly lower in SI patients (7.7 vs. 8.7, p<0.001). The BMQ domains “overuse” and “harm” did not differ significantly between the groups after multiple-testing correction (Figure).
Conclusions
Patients with SI had lower perceived necessity and fewer concerns regarding medicines than patients with other chronic diseases in general practice, while the Necessity-Concerns-Differential was also significantly lower. Within the cohort of statin-intolerant patients, lower NCD values were associated with less frequent lipid-lowering therapy and lower LDL-C target attainment. These findings highlight that cognitive and perceptual factors might contribute to treatment gaps in lipid management. Educational interventions addressing beliefs about medicines, especially its necessity, may improve lipid-lowering therapy utilization and medication adherence in patients with SI, particularly in those with low NCD.