Introduction As medicine becomes increasingly digital, patients must possess sufficient digital health literacy (dHL) to engage effectively in their care. In Germany, statutory health insurers are obliged to offer dHL education, yet little is known about the levels and social determinants of dHL in cardiac patients, or about their awareness of available training.
Methods Between July 2024 and April 2025, an anonymized cross-sectional survey was conducted across 14 outpatient clinics at the University Hospital Würzburg. This analysis focuses on participants recruited from the Comprehensive Heart Failure Cente (CHFC), Würzburg. Data collected from respondents included sociodemographic characteristics, dHL measured by the GR-eHEALS questionnaire (range 1–5), knowledge of and attitudes towards insurer funded dHL programs. Differences between dHL subgroups were tested using independent t-tests and linear regression (p for trend). Age- and sex-adjusted predictors of `low dHL´ (GR-eHEALS score <3) were analyzed using logistic regression.
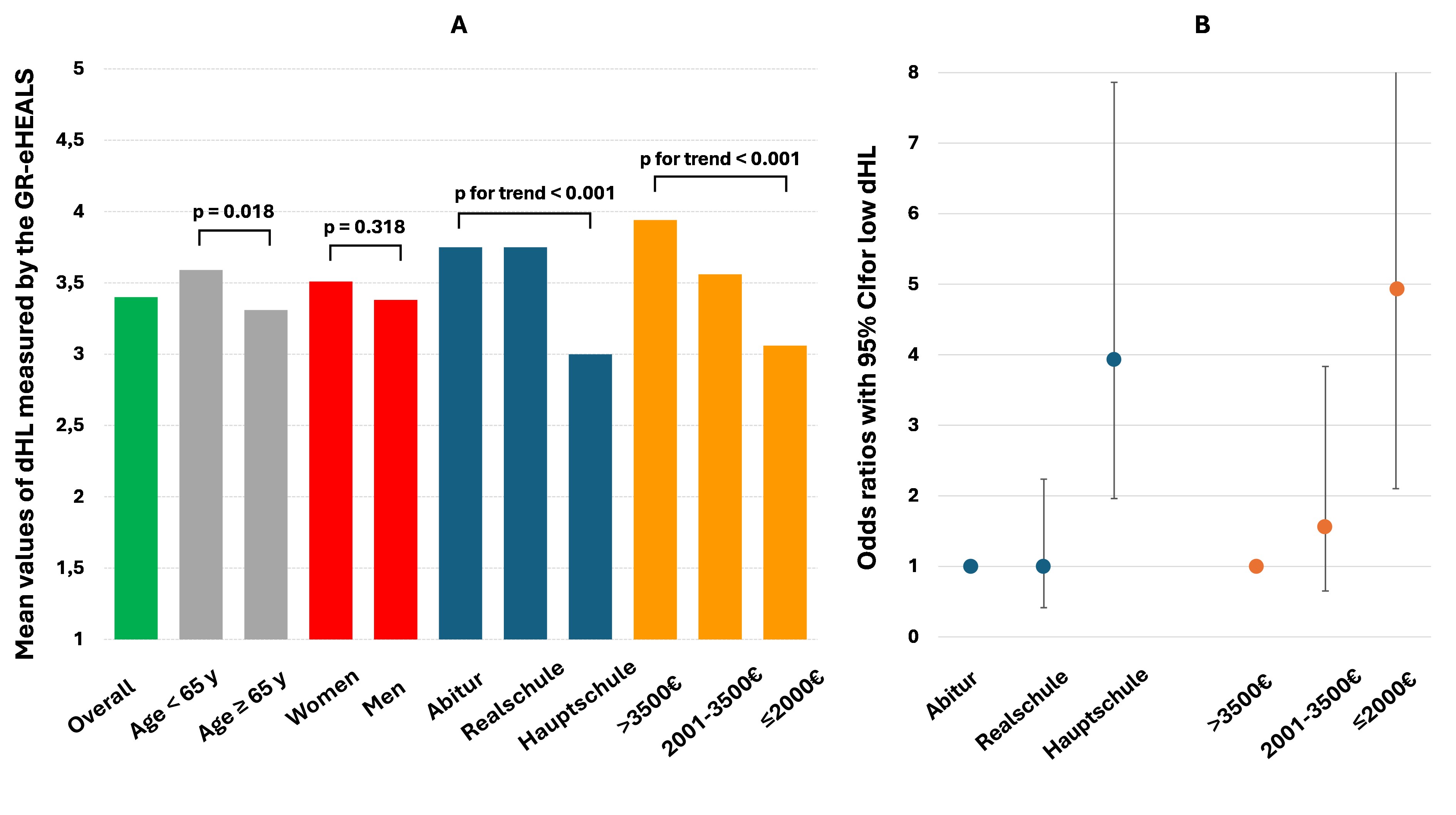
Results Of the 1,626 patients enrolled in the overall study, 255 from the CHFC outpatient clinic were included in the present analysis. Their mean age was 63 ± 16 years, and 35% were women. The mean dHL score was 3.4 ± 1.0. Patients with lower educational attainment (“Hauptschule”: 3.0 ± 1.1) and lower monthly income (<€2,000: 3.1 ± 1.1) showed significantly lower dHL compared to those with higher education (“Abitur”: 3.8 ± 0.8) or higher income (>€3,500: 3.9 ± 0.8) (Figure 1A). In multivariable models adjusting for age and sex, lower education (OR 3.9, 95 % CI 2.0 – 7.9) and low income (OR 4.9, 95 % CI 2.1 – 11.5) independently predicted low dHL (Figure 1B). Only 27 % of participants were aware of their insurer’s training programs, and 12 % had ever participated. Awareness and participation were lower among groups with lower education (“Hauptschule” vs. “Abitur”: 26% vs. 28% and 9% vs. 14%) and lower income (<€2,000 vs. >€3,500: 23% vs. 31% and 9% vs. 19% respectively). The overall willingness to participate in dHL training programs was 34%.
Conclusion Digital health literacy among cardiology outpatients is unevenly distributed: individuals with lower socioeconomic resources not only demonstrate lower dHL but are less likely to know about or attend existing training. Targeted outreach and accessible, patient-centered educational initiatives are needed to promote equitable engagement with digital cardiovascular care.