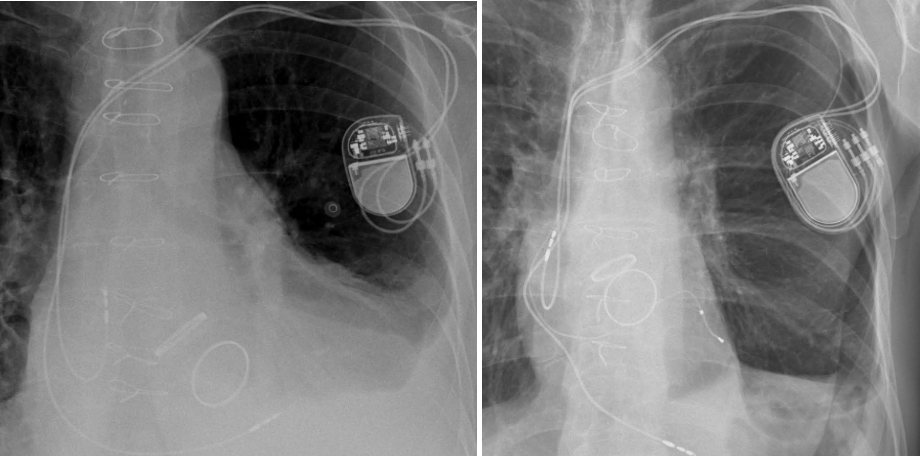
Background/Introduction
Atrioventricular and intraventricular conduction disturbances are common complications following valve surgery. Right ventricular pacing in patients with reduced ejection fraction is associated with worsening heart failure, increased hospitalizations, and higher mortality. However, postoperative reductions in ejection fraction can be transient. Furthermore, surgical alterations of cardiac anatomy may complicate the implantation of a coronary sinus lead or left bundle branch area pacing (LBBAP) lead.
Purpose
To evaluate the acute and long-term outcomes of left bundle branch area pacing (LBBAP) and cardiac resynchronization therapy (CRT) via the coronary sinus in patients after valve surgery.
Methods
We conducted a retrospective analysis of consecutive patients who underwent valve surgery (aortic, mitral, or tricuspid valve repair or replacement, with or without coronary artery bypass grafting) and subsequently received either CRT with a coronary sinus lead or LBBAP between January 2010 and July 2025. Baseline characteristics, procedural details, and clinical outcomes were assessed, including left ventricular ejection fraction (LVEF), degree of valve regurgitation before device implantation, and ECG parameters such as left ventricular activation time (LVAT), interpeak interval (for LBBAP), and QRS duration. Differences of procedural and follow-up parameters were investigated with a two-sided students’ t-test, a p value <0.05 was considered significant.
Results
A total of 178 consecutive patients were included (117 CRT and 61 LBBAP; 57 with an ICD system). The mean age was 69.8 ± 11.5 years, 129 (70.1%) were male, 49 (26.6%) had coronary artery disease, and mean LVEF was 37.5 ± 9.1%.
Fluoroscopy duration was 9.7 ± 11.6 minutes for CRT and 8.1 ± 4.3 minutes for LBBAP (p=0.94). Fluoroscopy dose was 660 ± 1194 cGy/cm² for CRT and 867 ± 1074 cGy/cm² for LBBAP (p=0.87). Paced QRS duration was comparable between CRT and LBBAP patients (159.1 ± 27.4 ms for CRT and 164.4 ± 28.1 ms (stimulus) / 133.0 ± 21.6 ms (deflection) for LBBAP, p=0.40 for paced QRS durations). In the LBBAP group, mean LVAT was 83.3 ± 15.8 ms and the V6/V1 interpeak interval was 40.7 ± 8.0 ms.
Median follow-up duration was 324 days (interquartile range, 108–736 days). LVEF improved from 33.6 ± 9.6% to 36.8 ± 12.1% in CRT patients and from 36.3 ± 9.9% to 43.9 ± 11.9% in LBBAP patients (p=0.03 for LVEF at end of follow-up). Progression of tricuspid regurgitation occurred in one CRT patient and in none of the LBBAP patients.
Conclusions
LBBAP may represent a reasonable alternative to CRT in patients with previous surgical valve repair or replacement, showing even better improvement in left ventricular ejection fraction during follow-up.