ImportanceDual antiplatelet therapy with P2Y
12 inhibitors is a cornerstone of secondary prevention after acute myocardial infarction. Yet, contemporary utilization patterns and the influence of evolving clinical guideline recommendations remain poorly characterized, and comparative data between continents are lacking.
ObjectiveTo describe utilization trends of P2Y
12 inhibitors in Germany vs the US between 2011 and 2024.
Design, Setting, ParticipantsA descriptive cohort study using longitudinal, nationwide health insurance claims from Germany (BARMER) and the US (Optum, MarketScan). The two country-specific cohorts included patients aged 18 years or older who were newly prescribed P2Y
12 inhibitors within 30 days of acute myocardial infarction.
InterventionsExposure to the P2Y
12 inhibitors clopidogrel, ticagrelor, and prasugrel, of which ticagrelor and prasugrel are considered high potent.
Main Outcomes and MeasuresThe primary outcome was the proportion and change in clopidogrel, ticagrelor or prasugrel users among patients newly prescribed P2Y
12 inhibitors in the outpatient setting during the 14-year observation period. Secondary outcomes included the proportion of patients filling P2Y
12 inhibitors within a week after hospital discharge.
ResultsDuring the study period, 162,314 German patients (mean [SD] age, 69.6 [12.9] years; 61.8% male) and 239,226 US patients (mean [SD] age 65.0 [12.4] years; 67.4% male) with comparable baseline characteristics received P2Y
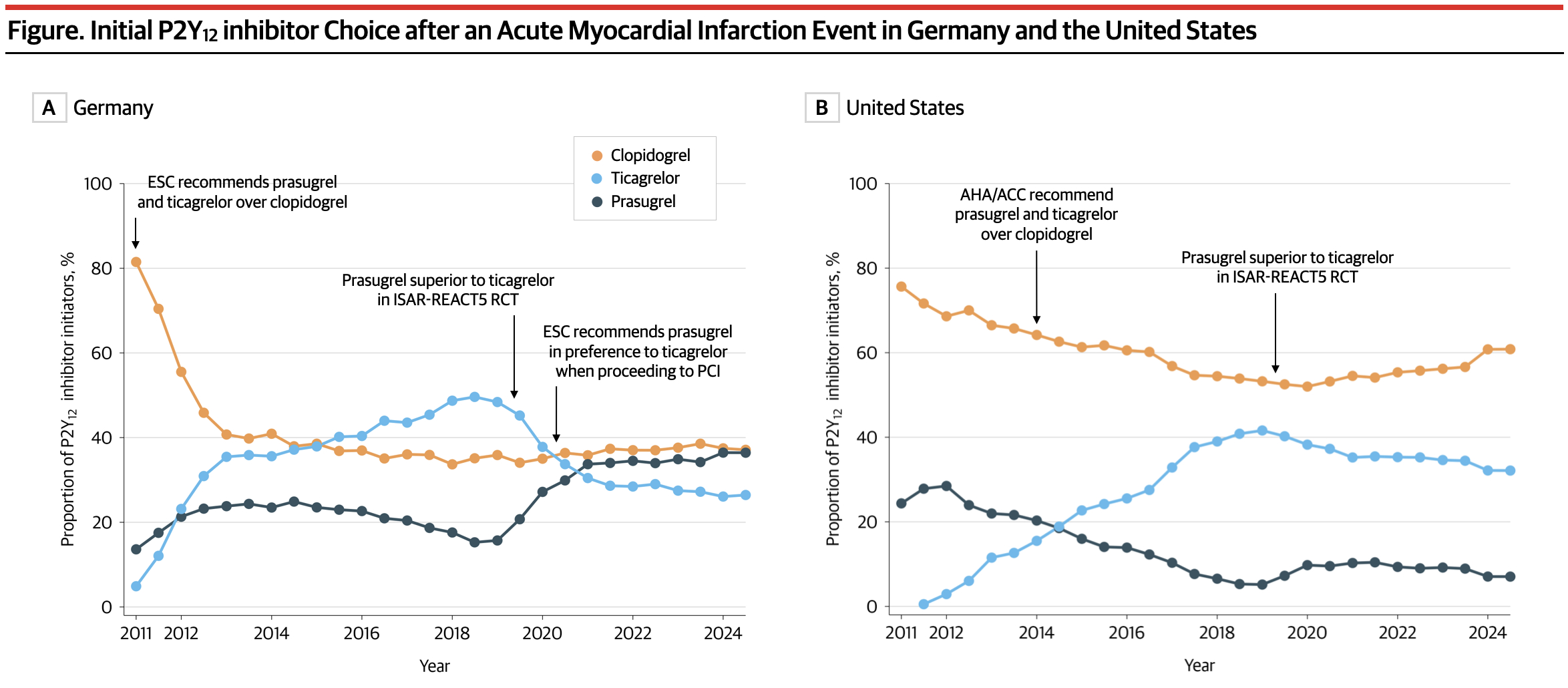
12 inhibitor therapy after acute myocardial infarction. From 2011 to 2024, clopidogrel use declined by 39% in Germany and 13% in the US, while ticagrelor use increased steadily through 2018 by 41% and 40%, respectively, consistent with regional guideline recommendations favoring potent P2Y
12 inhibitors since 2011 in Europe and 2014 in the US. Following the 2019 ISAR-REACT5 trial and European guideline recommendations favoring prasugrel over ticagrelor, the proportion of prasugrel users in Germany increased by 18%, with a corresponding 20% decline in ticagrelor use. In contrast, guideline recommendations in the US remained largely unchanged, and only modest changes in P2Y
12 inhibitor use were observed (prasugrel +5%, ticagrelor −9%). The proportion of patients filling a P2Y
12 inhibitor prescription within 7 days of hospital discharge was 89.2% in Germany vs 85.3% in the US.
Conclusion and RelevanceIn this study, use of the potent P2Y
12 inhibitors prasugrel and ticagrelor increased from 2011 to 2024 in both countries, with an earlier and steeper shift observed in Germany. These temporal differences appear to reflect variations in the timing and strength of regional guideline recommendations, with earlier and more specific European updates associated with greater changes in use. Despite broadly similar patient populations, prescribing patterns diverged substantially, suggesting that emerging evidence is interpreted and implemented differently across regions, with potential implications for achieving optimal patient care in a globalized evidence environment.