Importance
Heart failure represents the leading cause of hospital admissions in Germany. However, patterns of medications proven effective in patients with heart failure in the period surrounding hospitalization remain poorly understood.
Objective
To assess medication use before, during, and after hospitalization for heart failure and identify patient characteristics associated with the filling of prescriptions in the post-discharge period.
Design, Setting, and Participants
This population-based cohort study used nationwide German claims data (BARMER) from July 1, 2023, through June 30, 2024. Medication use of individuals hospitalized for heart failure was analyzed 91 days before, at discharge (≤91 days), and 92 to 183 days after hospitalization.
Main Outcomes and Measures
Prescription fills before and after hospitalization for heart failure were examined for the following medication classes: angiotensin-converting enzyme inhibitors (ACEIs), angiotensin receptor blockers (ARBs), angiotensin receptor neprilysin inhibitors (ARNIs), beta-blockers, mineralocorticoid receptor antagonists (MRAs), loop diuretics, sodium-glucose cotransporter 2 inhibitors (SGLT2i), and glucagon-like peptide-1 (GLP-1) receptor agonists. Modified Poisson regression with robust variance estimation was used to examine predictors of filling a prescription.
Results
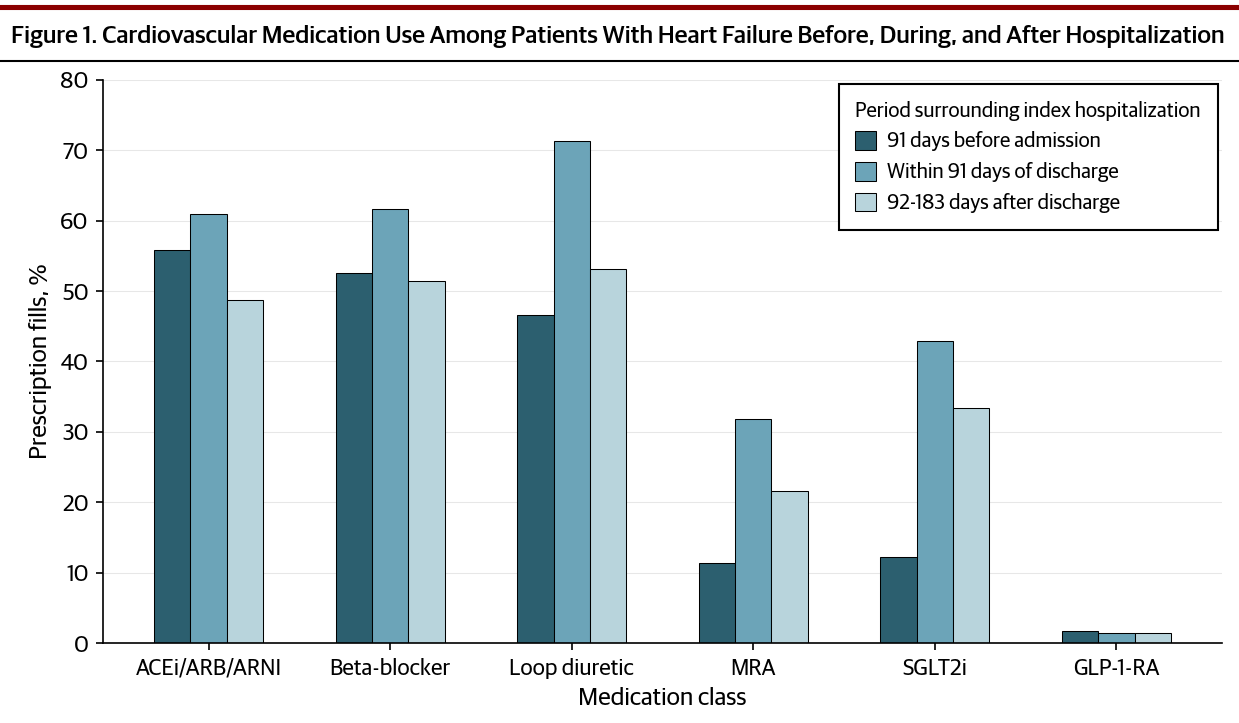
Among 31,708 patients hospitalized for heart failure (median age, 83 years (IQR, 75-88); 57.7% female), prescription fills increased for all classes except GLP-1 receptor agonists at discharge. The proportion of patients filling SGLT2 inhibitors rose the most from before hospitalization to discharge (12.3% to 42.8%), followed by loop diuretics (46.6% to 71.3%), MRAs (11.3% to 31.8%), beta-blockers (52.5% to 61.7%), and ACEIs/ARBs/ARNIs (55.8% to 60.9%). The factor with the largest point estimate for filling a prescription in the post-discharge period was having a prescription before hospitalization. Age showed a graded association with lower medication refills compared with patients in the age group of 18-64 years, those aged 65-74, 75-84, and ≥85 years were less likely to fill a prescription after discharge with the largest reductions observed for ACEIs/ARBs/ARNIs (ARR, 0.92 [95% CI 0.88-0.95], 0.86 [95% CI 0.83-0.89], and 0.76 [95% CI 0.73-0.79], respectively). Among healthcare use factors, cardiologist visits were associated with higher initiation rates, with the strongest effect for SGLT2i (ARR 1.06 [95% CI 1.03-1.10]).
Conclusions and Relevance
The use of common heart failure therapies temporarily increased after hospitalization for heart failure, and declined within six months post-discharge. Incomplete implementation of effective heart failure therapies highlights the need to improve post-discharge medication management in individuals with heart failure.