Aims/Introduction:
Recent studies have demonstrated that heart-reactive autoantibodies (HRA) may occur not only in cardiac disease but also in the general population. While HRAs are often considered pathogenic regarding cardiac function, their role in psychological well-being and self-perceived health remains unclear. We hypothesised that HRAs may indicate a certain degree of chronic inflammation, which potentially influences brain function and promotes inflammation-associated distress. We therefore examined the association between HRA serum levels and self-rated health and anxiety.
Methods:
We analysed serum samples from 601 adults (30–79 years, 58% female), a representative sub-sample of the population-based STAAB cohort (Characteristics and Course of Heart Failure Stages A–B and Determinants of Progression, Würzburg, Germany). Using bead-based flow cytometric assays, we quantified autoantibody reactivities against cardiac proteins (2nd extracellular loop of the β1-adrenergic receptor (β1AR-ECII), Troponin I3 (TPI3), Tropomyosin 1 (TPM1), Myosin Heavy Chains 6 and 7 (MYH6, MYH7), and Myosin Light Chain 7 (MYL7)). Associations with self-reported health (EQ-5D visual analogue scale) and anxiety symptoms (GAD-7) were assessed using multivariable models adjusted for age and sex.
Results:
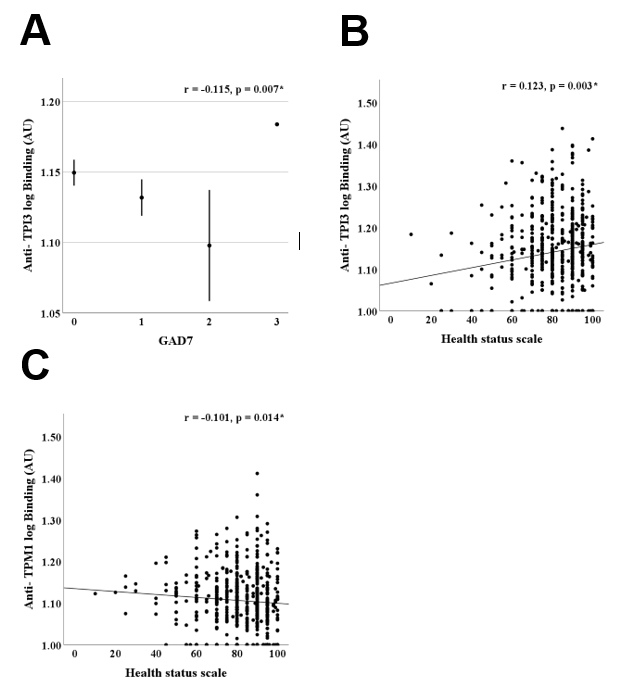
Higher anti-TPI3 antibody levels were significantly associated with lower anxiety scores (Fig. A) and better self-rated health (Fig. B), whereas higher amounts of HRA against TPM1 were linked to poorer self-rated health (Fig. C). These associations remained statistically significant after adjustment for age and sex. No significant associations between self-reported health and HRA levels were observed for antibodies against β1AR-ECII, MYH6, MYH7, or MYL7.
Conclusion:
In this population-based sample free from overt heart failure, distinct HRA profiles were associated with psychological well-being. Specifically, anti-TPI3 antibody levels were positively correlated with better self-perceived health and lower anxiety, whereas higher anti-TPM1 antibody levels indicated reduced health perception. These findings suggest that selected HRAs may reflect aspects of cardiovascular and psychological resilience rather than disease, highlighting their potential role as biomarkers of well-being and good prognosis in preventive cardiology.