Background
Systemic inflammation is a key pathophysiological driver of arterial events and major adverse cardiovascular and cerebrovascular events (MACCE). Pyoderma gangrenosum (PG), a rare neutrophilic dermatosis, is characterized by marked systemic inflammatory activity. This study aimed to assess whether PG is associated with an increased risk of arterial events and MACCE compared with individuals without PG.
Methods
Data were obtained from TriNetX, a global federated network of anonymized electronic health records used for large-scale real-world analyses. PG patients without preexisting atherosclerotic disease were compared with a PG-free patient cohort and the outcome was assessed over a 5-year follow-up period with respect to MACCE, defined as all-cause death, cardiac arrest, cardiogenic shock, myocardial infarction (MI), stroke and acute heart failure. Secondary analysis included assessment of the separate risk for following endpoints: all-cause mortality, MI, ischemic stroke and clinically relevant peripheral artery disease (PAD). Multivariable Cox regression analysis was performed after adjustment for age, demographics, socioeconomic status, diabetes mellitus, obesity, hypertension, noninfective enteritis and colitis, inflammatory polyarthropathies, neoplasms, and immunosuppressive medication.
Results
A total of 3 093 204 subjects was analyzed consisting of 12194 PG patients. PG patients were more frequently female (65.1% vs. 49.8%; p < 0.001), had a higher cardiovascular risk burden including hypertension (27.4% vs. 13.4%; p < 0.001), diabetes (13.3% vs. 5.6%; p < 0.001), obesity (17.3% vs. 10.7%; p < 0.001), and chronic kidney disease (5.6% vs. 1.7%; p < 0.001). However, LDL-C levels were modestly lower in PG (97.9 ± 37.2 vs. 104.5 ± 34.9 mg/dL; p < 0.001).
Using a cox regression analysis, PG was independently associated with a 61% higher risk of MACCE (HR 1.61; 95% CI 1.53–1.70; p < 0.001), a 43% higher risk of MI (HR 1.43; 95% CI 1.28–1.61; p < 0.001), and a 17% higher risk of stroke (HR 1.17; 95% CI 1.06–1.30; p = 0.004). The association with symptomatic PAD was particularly pronounced (HR 4.50; 95% CI 3.99–5.08; p < 0.001) (Figure 1). Sensitivity analyses (same model, 90-day washout; risk window day 90–1,825) confirmed the robustness of the findings.
Conclusions
In this large real-world cohort, we identified for the first time that PG being associated with a significantly increased risk of major cardiovascular events. These findings support recognizing PG as a clinically relevant systemic inflammatory cardiovascular risk factor and underscore the importance of implementing aggressive primary prevention strategies in this patient population.
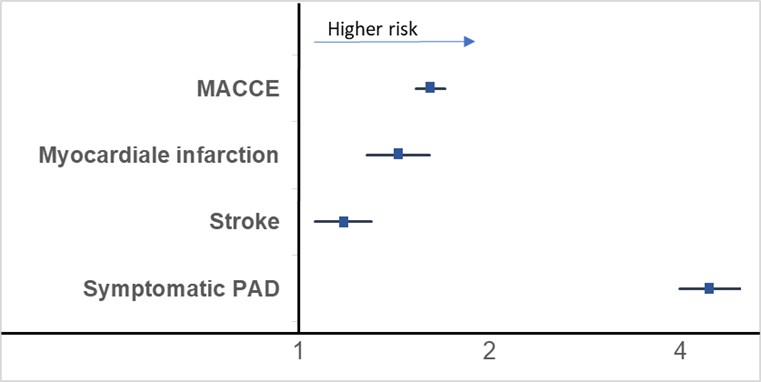
Figure 1: Multivariable Cox Regression Analysis of Cardiovascular Endpoints in Pyoderma Gangrenosum
