Background:
Most data on the prevalence of left atrial thrombus (LAT) detected by transesophageal echocardiography (TEE) were published 10 to 30 years ago. Since then, the widespread use of direct oral anticoagulants and substantial improvements in echocardiographic image quality are likely to have influenced LAT prevalence. At the same time, emerging transthoracic echocardiographic parameters reflecting left atrial cardiomyopathy (LA-CMP) may serve as predictors of LAT formation. Therefore, we aimed to assess the current prevalence of LAT in a contemporary, unselected cohort undergoing TEE for any indication at a large tertiary care center. In addition, the presence or absence of LA-CMP, as determined from same-session transthoracic echocardiographic (TTE) imaging, was correlated with TEE findings.
Methods:
In this retrospective study, we included all consecutive patients who underwent same-session TTE and TEE between July 2020 and July 2025. To ensure consistency in acquisition and imaging parameters, only studies performed by a single experienced operator (MSR) were analyzed. All examinations were re-evaluated by an independent expert observer (HR). The presence and grade of spontaneous echo contrast (SEC 1–4), sludge, and thrombus in the left atrial appendage (LAA) were documented. Each TEE study also included dedicated 0° and 90° sweeps of the left atrium to detect thrombi outside the appendage. Left atrial thrombotic substrate (LATS) was defined as SEC grade 4, sludge, or thrombus within the left atrium or LAA.
For all patients, same-session TTE images were analyzed to quantify left atrial reservoir (LASr), conduit (LAScd), and contraction strain (LASct) as surrogates of left atrial cardiomyopathy (LA-CMP). The presence of LATS was then correlated with indices of LA-CMP.
Results:
A total of 2,712 patients were included in the final analysis. Of these, 58% were male, and the mean age was 66 ± 15 years. The mean left ventricular ejection fraction (LVEF) was 55 ± 11%, and 1,134 patients (41.8%) had at least moderate valvular heart disease. A left atrial appendage (LAA) thrombus was detected in 106 patients (3.9%), while 18 patients (0.7%) demonstrated significant left atrial findings outside the LAA (thrombus or myxoma). A total of 364 patients (13,4%) showed LATS.
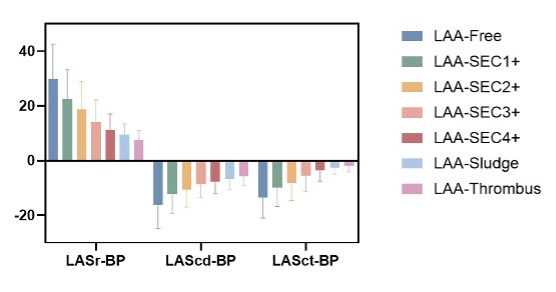
Left atrial strain parameters—reservoir (LASr), conduit (LAScd), and contraction (LASct) strain—were all significantly associated with the presence of LATS (Figure 1). In multivariable regression analysis, all three remained independent predictors of LATS after adjustment for left atrial volume, LVEF, and valvular heart disease.
Conclusion:
In this large contemporary hospital-based cohort representing a high-risk patient population, the prevalence of left atrial thrombotic substrate was 3.9% in the left atrial appendage and 0.7% in the remaining left atrium. Reduced left atrial strain, reflecting left atrial cardiomyopathy, was the only independent predictor identifiable from transthoracic echocardiographic parameters.
Figure 1: