Background: There is limited data to guide risk stratification, predict adverse events, and identify patients who will benefit from implantable cardioverter-defibrillator (ICD) therapy in Brugada syndrome (BrS), particularly among patients who are asymptomatic at diagnosis. Strikingly, in 4.6% of patients, sudden cardiac death (SCD) is reported to be the initial presentation of BrS, underlining the importance of proper risk stratification of the asymptomatic BrS population.
Objective: In our arrhythmia syndrome outpatient clinic, we evaluated whether specific predictors, including mode of diagnosis or symptom status at initial presentation, could stratify patients in regard to their risk of major arrhythmic events (MAE).
Methods: This single-center retrospective cohort study included 82 patients with BrS which presented from January 1995 to August 2021. MAE was the primary composite outcome, including sustained ventricular tachycardia (VT), ventricular fibrillation (VF), and sudden cardiac death (SCD), and was assessed along with potential clinical predictors of these events.
Results: In a total of 82 patients with documented type 1 Brugada ECG, a follow-up of 81±77 months was performed. Overall, MAE occurred in 16/82 (19.5%) patients. Among a subgroup of 62 patients who had a follow-up period over >12 months, MAE occurred in 11/62 (17.7%) patients, resulting in an annual event rate of 2.0% (vs. 2.8% in the whole cohort).
In the full cohort, documented non-sustained VT (nsVT) and symptoms at diagnosis were the only significant predictors of MAE during follow-up. Patients with a history of nsVT had a substantially increased risk of MAE during follow-up (OR 9.5, 95% CI 2.0-45.8, p=0.005; Fig.1B). Patients who were symptomatic at diagnosis (syncope or documented arrhythmia either nsVT or MAE as defined above) had a markedly higher lifetime risk of MAE than those patients that were diagnosed incidentally or through family screening (OR 6.9, 95% CI 1.4-34.8, p=0.019, Fig.1A). Patients who were asymptomatic at the time of diagnosis, however, showed a non‑significant protective trend (OR 0.3, CI 0.1-1.7, p = 0.19).
Conclusion: Non-sustained VT or symptoms at diagnosis seem to predict adverse outcome in patients with BrS. A trend towards improved outcomes among asymptomatic patients at diagnosis conflicts with a previously reported relevant number of SCD in asymptomatic BrS patients, illustrating the need for better risk stratification, specifically in this group of patients.
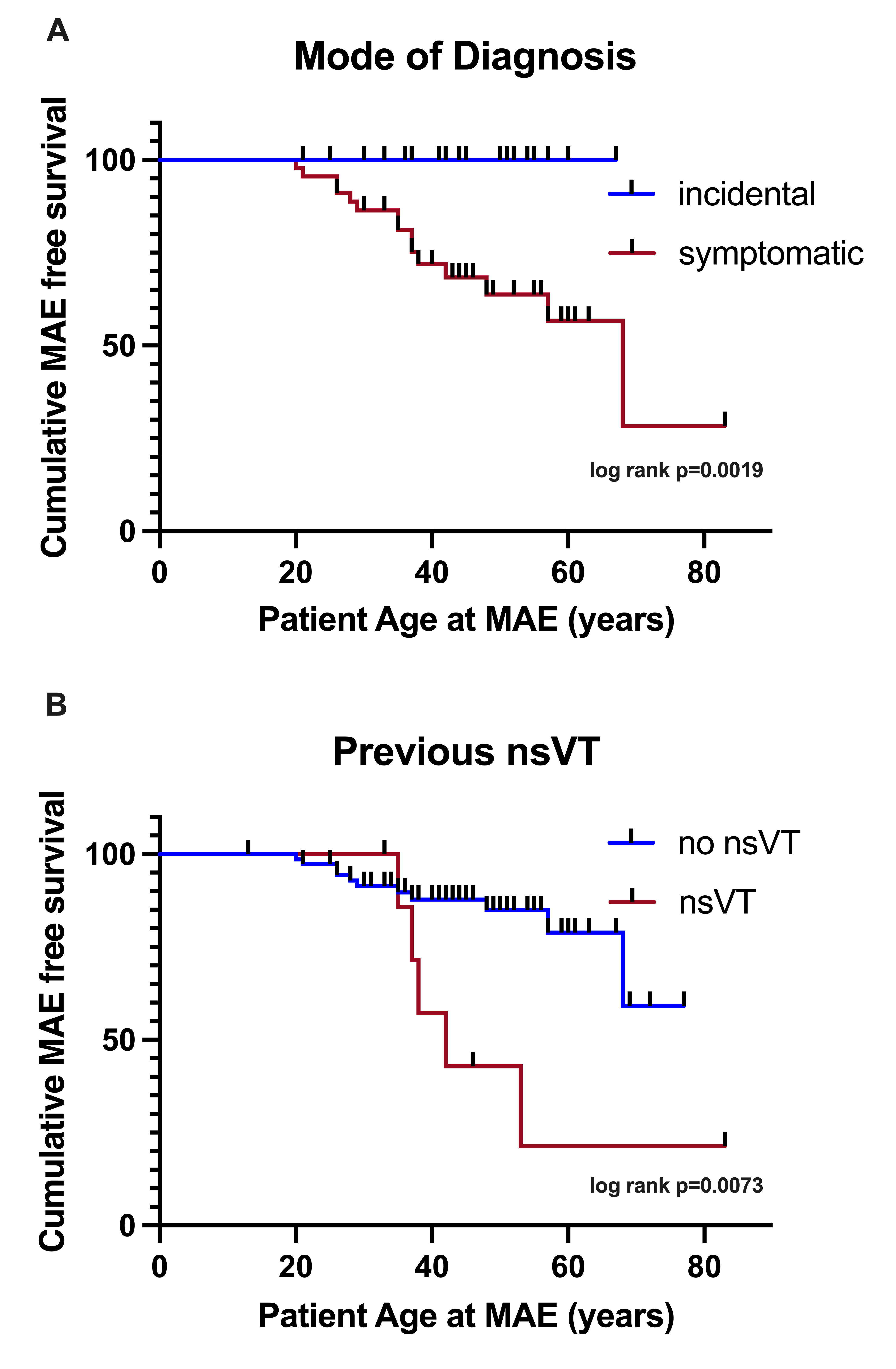
Figure 1. Cumulative MAE free survival stratified by mode of diagnosis (log-rank p = 0.0019; A) or by previous occurrence of nsVT (log-rank p = 0.0073; B). Patients diagnosed incidentally are shown in blue, patients diagnosed after symptoms are shown in red.
