Abstract:
Background: Left atrial (LA) linear ablation is either used as an adjunct to pulmonary vein (PV) isolation or frequently required to treat subsequent LA tachycardia since the majority of these arrhythmias underlie a macro-reentrant mechanism. High-power short-duration (hPSD) and ablation index (AI)-guided approaches are two widely adopted methods, yet direct comparisons of their effectiveness and safety are limited.
Objective: This observational study aimed to evaluate the efficacy and complication rates of ahPSD approach (50W/15 seconds, Thermocool Smarttouch) versus AI-guided ablation strategies in linear lesion formation (30W or 35W with AI Index: 600 for anterior line and 500 for roof line) for persistent AF.
Methods: Data were analyzed from a cohort of 214 patients (58% male, 68 ± 8 years)undergoing catheter ablation for persistent AF at the university medical center Mainz from 2020 to 2023. The primary endpoints were acute procedural success (first-pass block and procedure time) and long-term freedom from AF recurrence. Secondary endpoints included complication rates, such as groin-related complications, cardiac tamponade, and stroke.
Results: The hPSD group (n=114) demonstrated comparable acute procedural success and long-term arrhythmia-free survival compared to the AI group (n=100). (figure1) However, hPSD was associated with a shorter procedural time (AI: 137 ± 31 vs. hPSD: 95.83 ± 32.14 min) and reduced fluoroscopy time (6.5 ± 3.8 vs. 5.6 ± 14.6 min). Complication rates, including major adverse events, were similar between groups (3% vs. 5%, p=0.5). First pass block was comparable for roof line (AI: 93% vs. HPSD: 87%, p=0.1) and anterior line (AI: 70% vs. HPSD: 74%, p=0.6).
Conclusion: Both hPSD and AI-guided strategies are effective and safe for linear lesion ablation in persistent AF. hPSD offers the advantage of procedural efficiency without compromising outcomes, suggesting its potential as a preferred approach in specific clinical scenarios. Further randomized studies are warranted to confirm these findings.
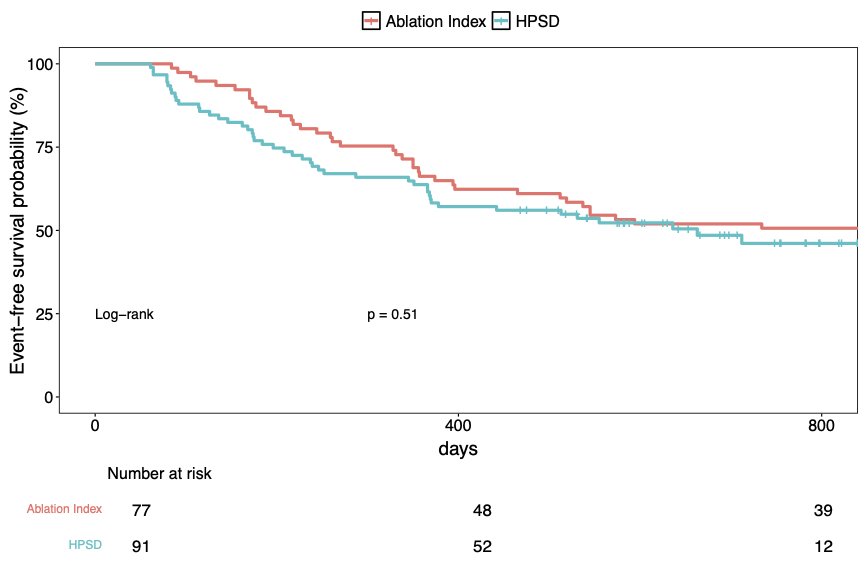
Figure1: Comparison of Ablation Index and High Power Short Duration ablation protocols during longterm follow-up.
