Background: Obstructive hypertrophic cardiomyopathy (HCM) is a chronic disease that reduces the quality of life. However, evidence regarding depression, anxiety, and socioeconomic risk factors among patients with obstructive HCM is limited. This study characterized the psychological burden in this population using statutory health insurance data and questionnaire-based assessments.
Methods: We evaluated data from the German Analysis Database for Evaluation and Health Services Research encompassing 4.4 million insured individuals between 2013 and 2023. Multivariable logistic regression identified characteristics associated with depression. Additionally, Patient Health Questionnaire-9 (PHQ-9) and Hospital Anxiety and Depression Scale (HADS) assessments were performed in 44 outpatients with obstructive HCM treated at a German tertiary care center.
Results: In the nationwide claims dataset, the prevalence of depression in obstructive HCM patients was 33.9%. Increased risk of depression was associated with older age (aOR 2.38; 95% CI 1.30–3.95) and female sex (aOR 2.06; 95% CI 1.88–2.26; both p < 0.001). Additional potential risk factors included receipt of unemployment benefits (aOR 2.19; 95% CI 0.78–1.25; p < 0.001), syncope (aOR 1.40; 95% CI 1.16–1.69; p < 0.001), and heart failure (aOR 1.20; 95% CI 1.08–1.32; p < 0.001). Beta-blocker (aOR 0.81; 95% CI 0.73–0.90; p < 0.01) and calcium-channel-blocker therapy (aOR 0.68; 95% CI 0.58–0.79; p < 0.001), German nationality (aOR 0.41; 95% CI 0.35–0.49; p < 0.001), and higher education level (aOR 0.67; 95% CI 0.44–1.01; p < 0.05) were associated with reduced risk (Table 1). These data were confirmed and extended using detailed questionnaires in patients with obstructive HCM. Clinically significant depressive symptoms were identified in 25.0% of patients using the PHQ-9 and 36.4% using the HADS-D; anxiety symptoms (HADS-A) were present in 20.5% (Figure 1). Higher NYHA class strongly correlated with PHQ-9 (ρ = 0.66), HADS-D (ρ = 0.64), and HADS-A scores (ρ = 0.53; all p < 0.001). PHQ-9 and HADS-D scores showed a strong correlation (ρ = 0.84; p < 0.001).
Conclusion: Depression and anxiety are common among patients with obstructive HCM in Germany and are closely linked to functional disease severity. Older individuals and women appear particularly vulnerable. Routine psychological screening may enhance comprehensive HCM care.
Table 1

Table 1. Statistically significant characteristics associated with depression.
Figure 1
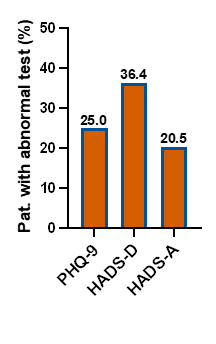
Figure 1. Fraction of patients with abnormal test scores in percentage.
