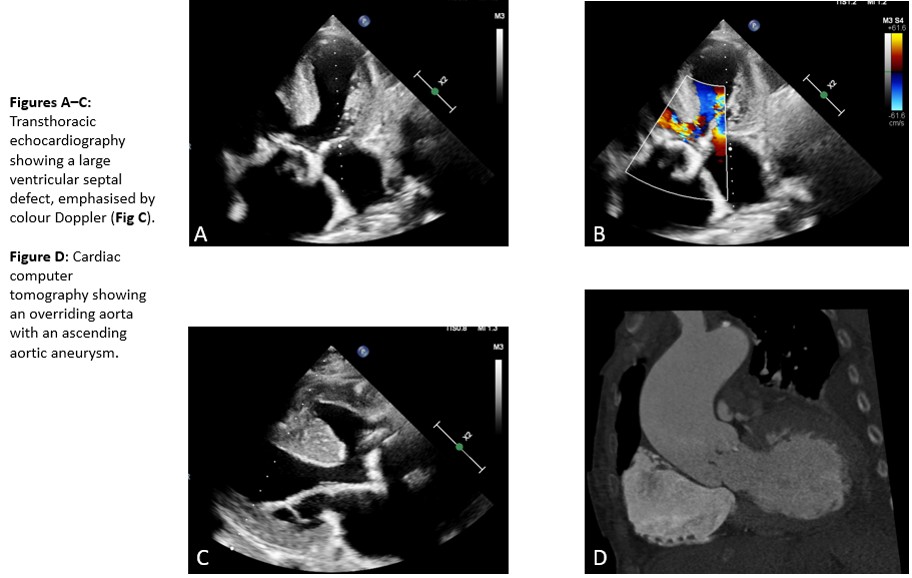
IntroductionTetralogy of Fallot (TOF) is the most common congenital heart defect with cyanosis, characterised by pulmonary stenosis, ventricular septal defect, right ventricular hypertrophy and an overriding aorta. Typically, TOF is treated surgically in the first year. Prognosis in uncorrected cases remains poor, with approximately half of patients dying in the first few years of life, with rare cases of patients living beyond the third decade.
We present the case of a 51-year old woman with unrepaired TOF, who presented with acute decompensated heart failure.
Clinical CaseA 51-year-old woman was found collapsed on the street and brought to our emergency department with severe cyanosis, dyspnoea and tachycardia. Due to a language barrier, a detailed medical history could not be obtained initially.
Echocardiography and cardiac CT revealed an unrepaired TOF with a subvalvular ventricular septal defect (2.4 cm), pulmonary stenosis or right ventricular outflow obstruction respectively, overriding aorta, and right ventricular hypertrophy. Additional findings included an aneurysm of the ascending aorta (5.7 cm), severe aortic stenosis with moderate regurgitation, and severe tricuspid regurgitation with bilateral pleural effusions. Coronary angiography excluded coronary artery disease. Laboratory testing showed elevated troponin (300,000 ng/L) and lactate (4 mmol/L). Staphylococcus saprophyticus was isolated from blood cultures, sensitive to initiated antibiotic therapy.
The patient was treated in the intensive care unit for six days with non-invasive assisted ventilation and respiratory support (HFNC), intravenous diuretics, and rate control for atrial tachyarrhythmia. On Day 4, a right-sided pleural drainage yielded 700 mL of fluid. After stabilisation and a significant reduction in NT-proBNP (15,000 → 8,800 ng/L), she was transferred to the intermediate care unit. Given severe comorbidities, noncompliance, lack of insurance, absence of social connections to relatives or friends and poor post-transplant prospects, heart–lung transplantation was deemed not feasible.
The patient self-discharged on Day 17 of hospitalisation, in chronically reduced, but stable cardiopulmonary condition. Four weeks later, she was readmitted after out-of-hospital cardiac arrest, and subsequently died from pneumonic sepsis.
ConclusionThis case illustrates an exceptional long-term survival of an adult with unrepaired Tetralogy of Fallot reaching the sixth decade of life. The patient’s outcome emphasizes the fragile balance in end-stage congenital heart disease and highlights the importance of coordinated multidisciplinary and social support structures, especially in vulnerable, uninsured adults with complex congenital heart defects.